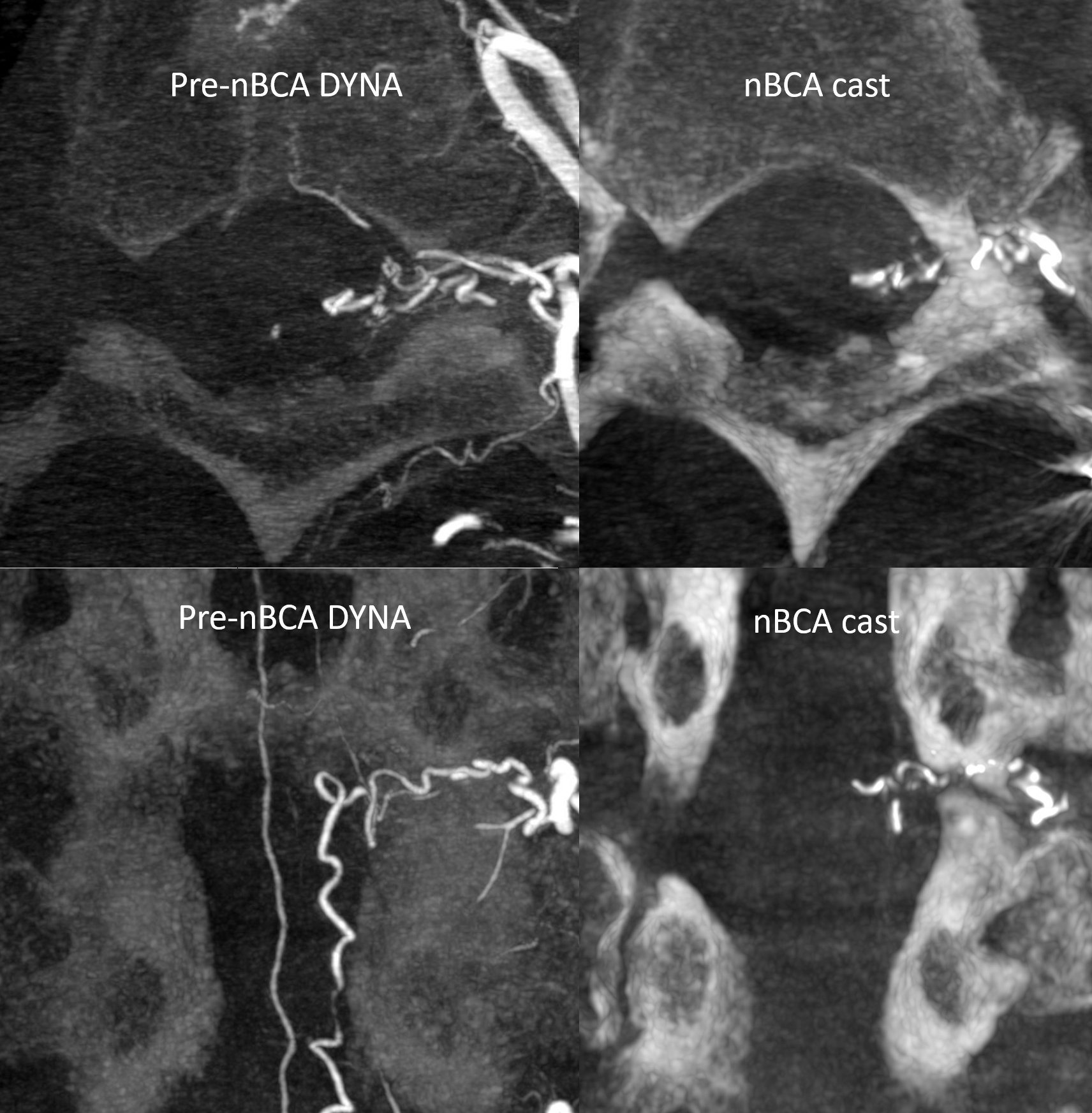
This case highlights some important spinal angiographic technique points. History is progressive lower extremity and bowel/bladder deficits. The patient had an abnormal MRI and a negative spinal angiogram. Two additional spinal angiograms followed, also negative, as well as more dedicated MRI / MRA scans. Extensive workup of alternative etiologies was also negative. Despite these setbacks and disease progression, the patient continued to look for a solution. The fistula was found on a 4th angiogram and closed by nBCA embolization. Below are images of the 4th angiogram, and at the end review of the first three.
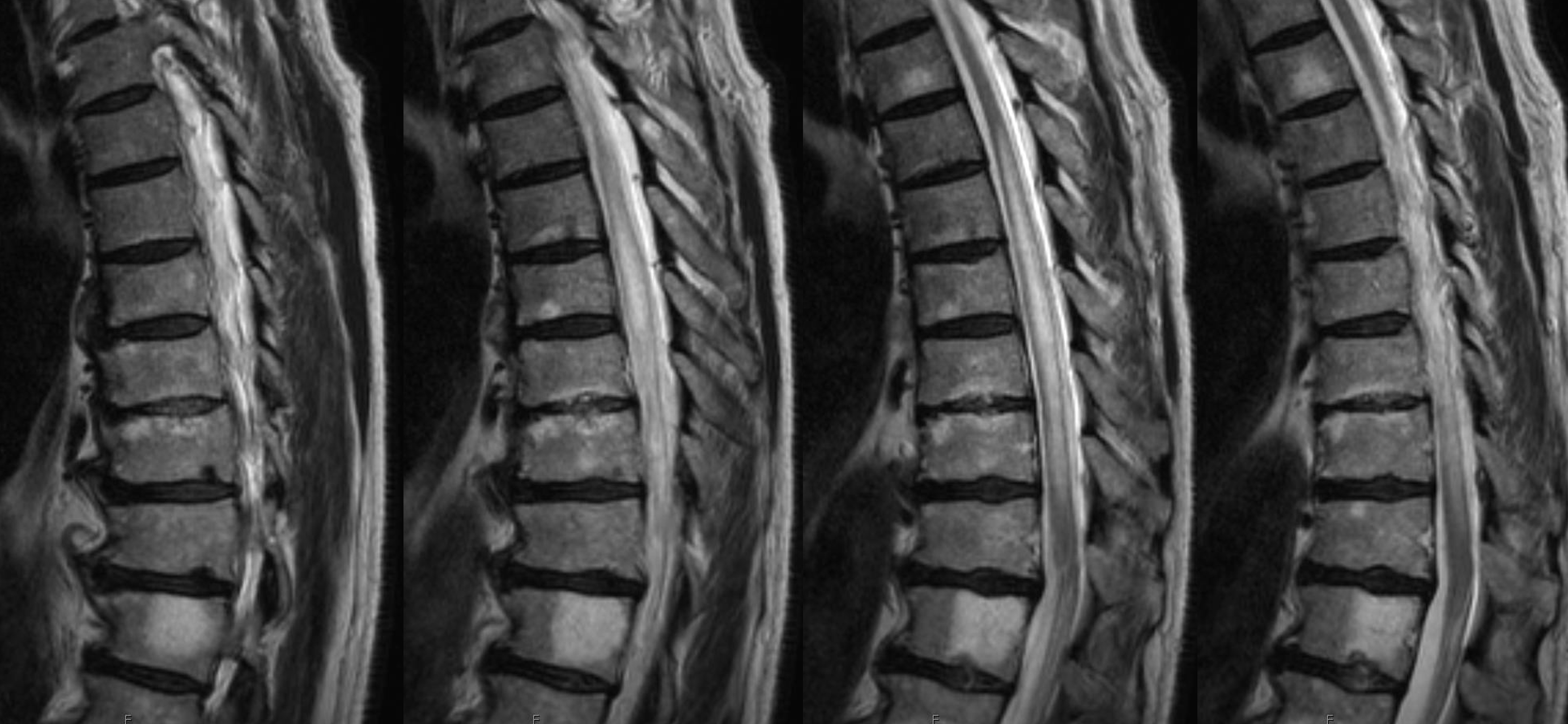
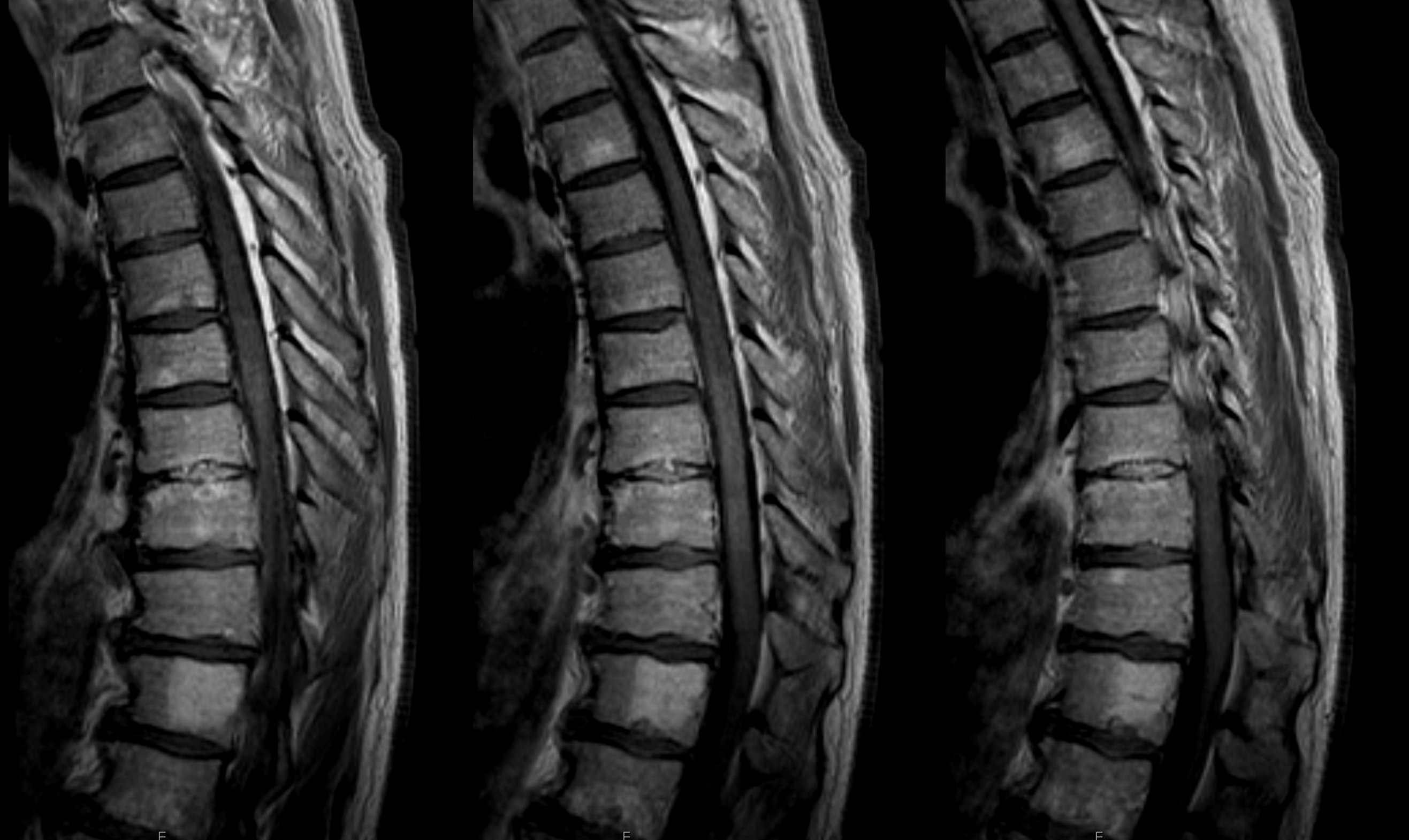
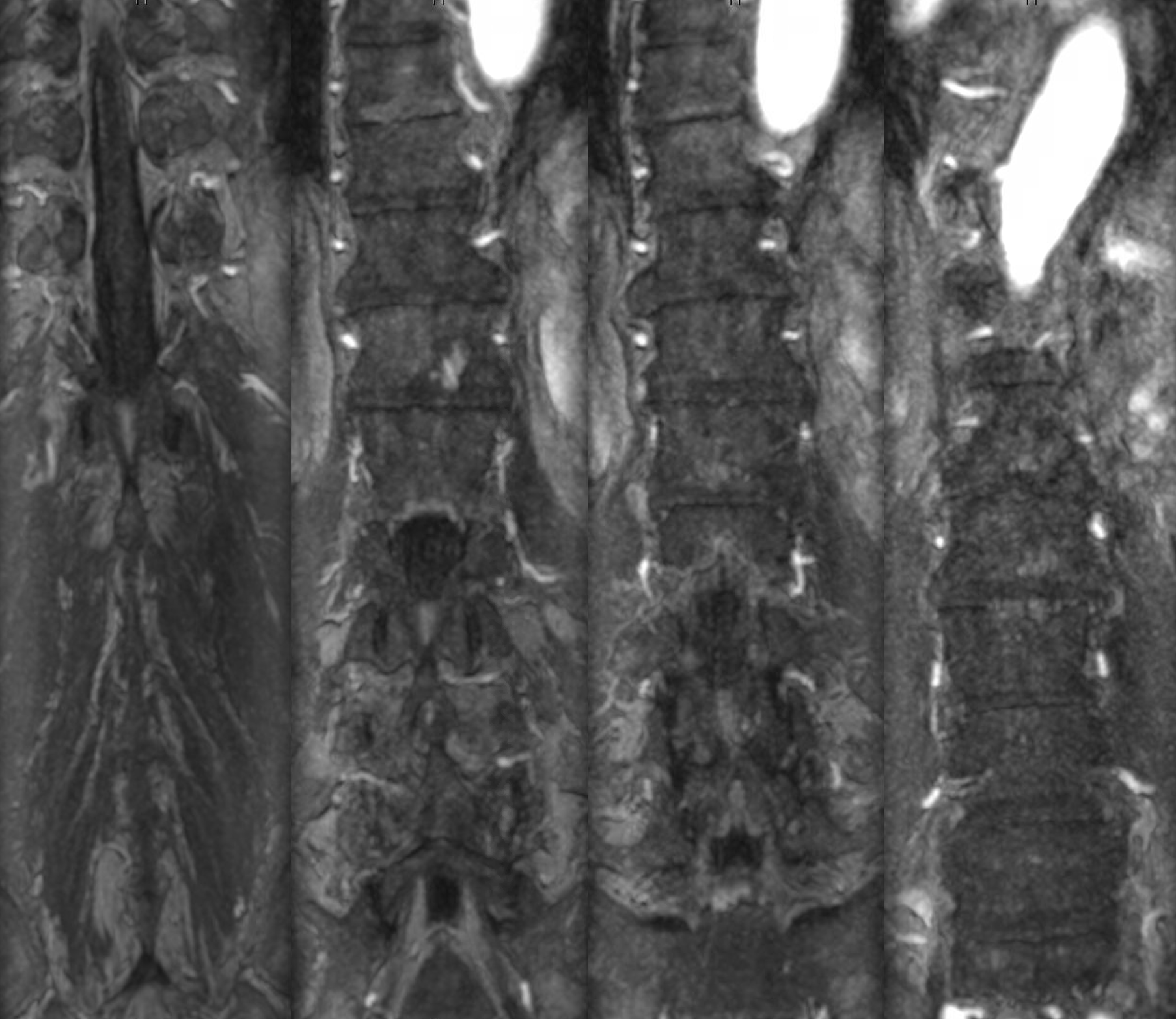
MRI — notice segmental edema — the conus region seems normal. This contributed to the uncertainty as to whether this was in fact a dural fistula. After 3 negative angiograms, I was not sure either.
Dedicated dynamic MRA. They do show fistula locations as often as not, the more the larger the fistulas are, and thus may spare some catheterizations. The issue in this case is that the fistula is likely very small. Modern dynamic MRA, though continuously improving, remains far below the required resolution. A high-res volumetric coronal T2 is probably much better.
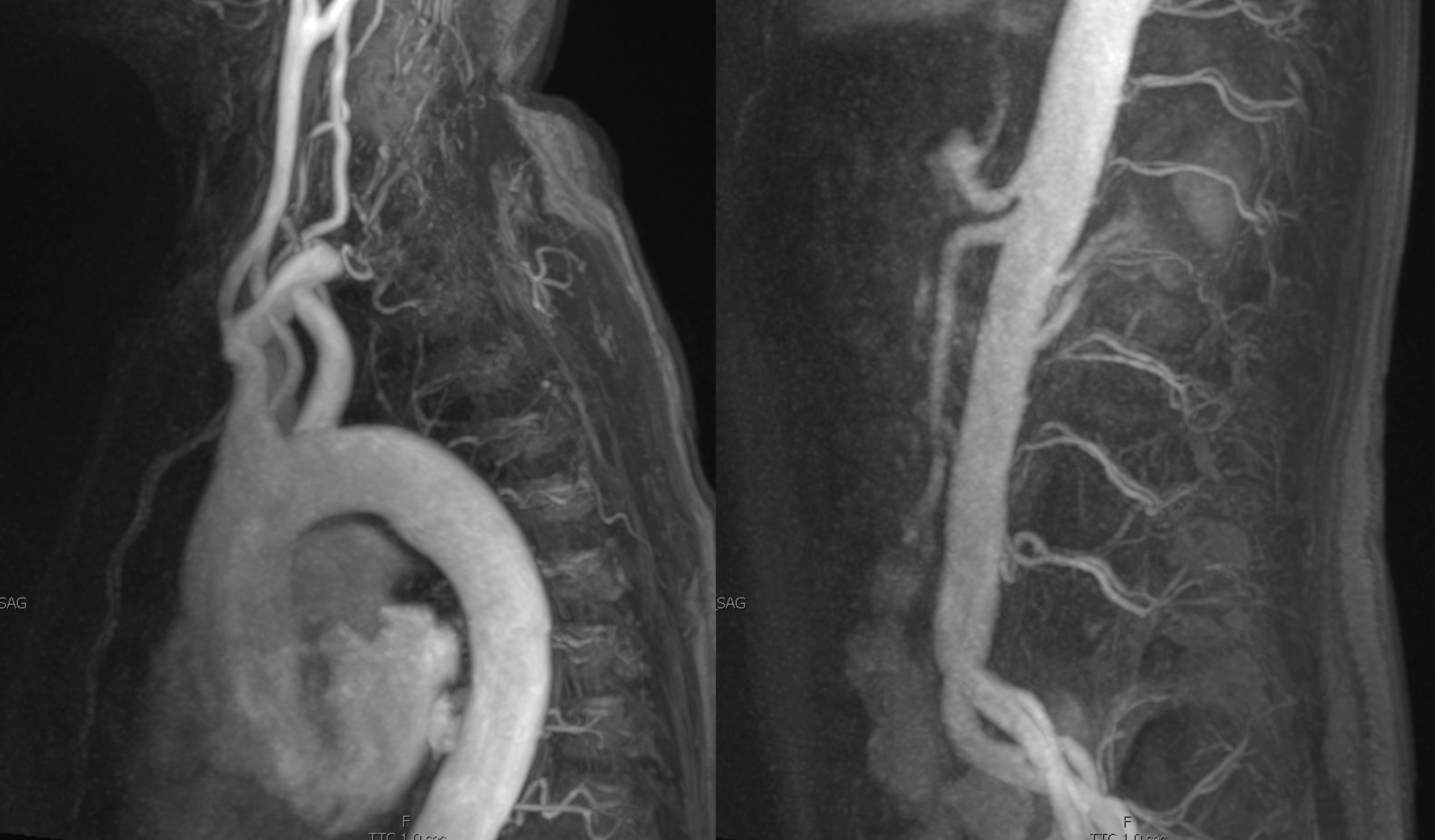
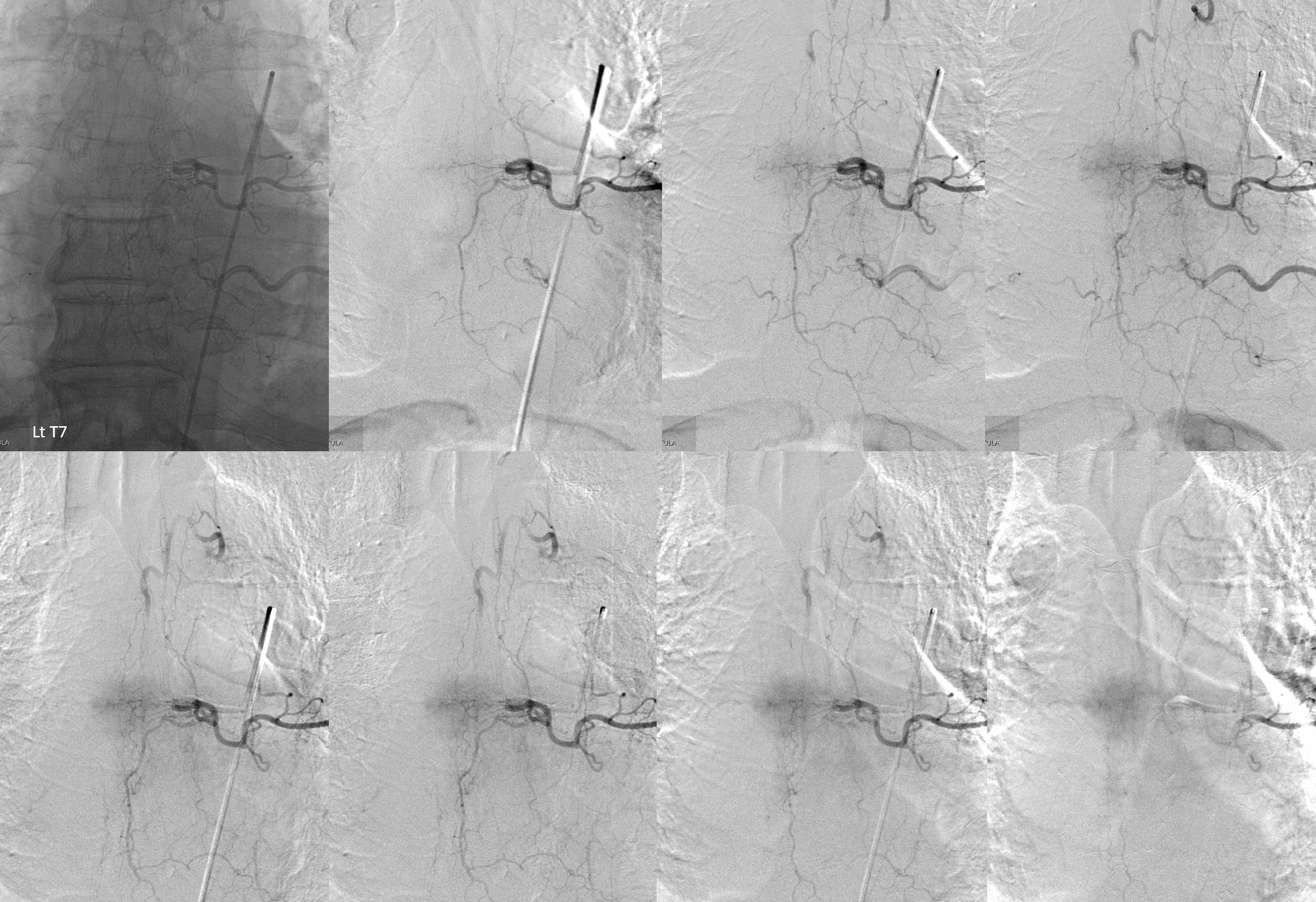
The fistula was found at left T7 level — see it?
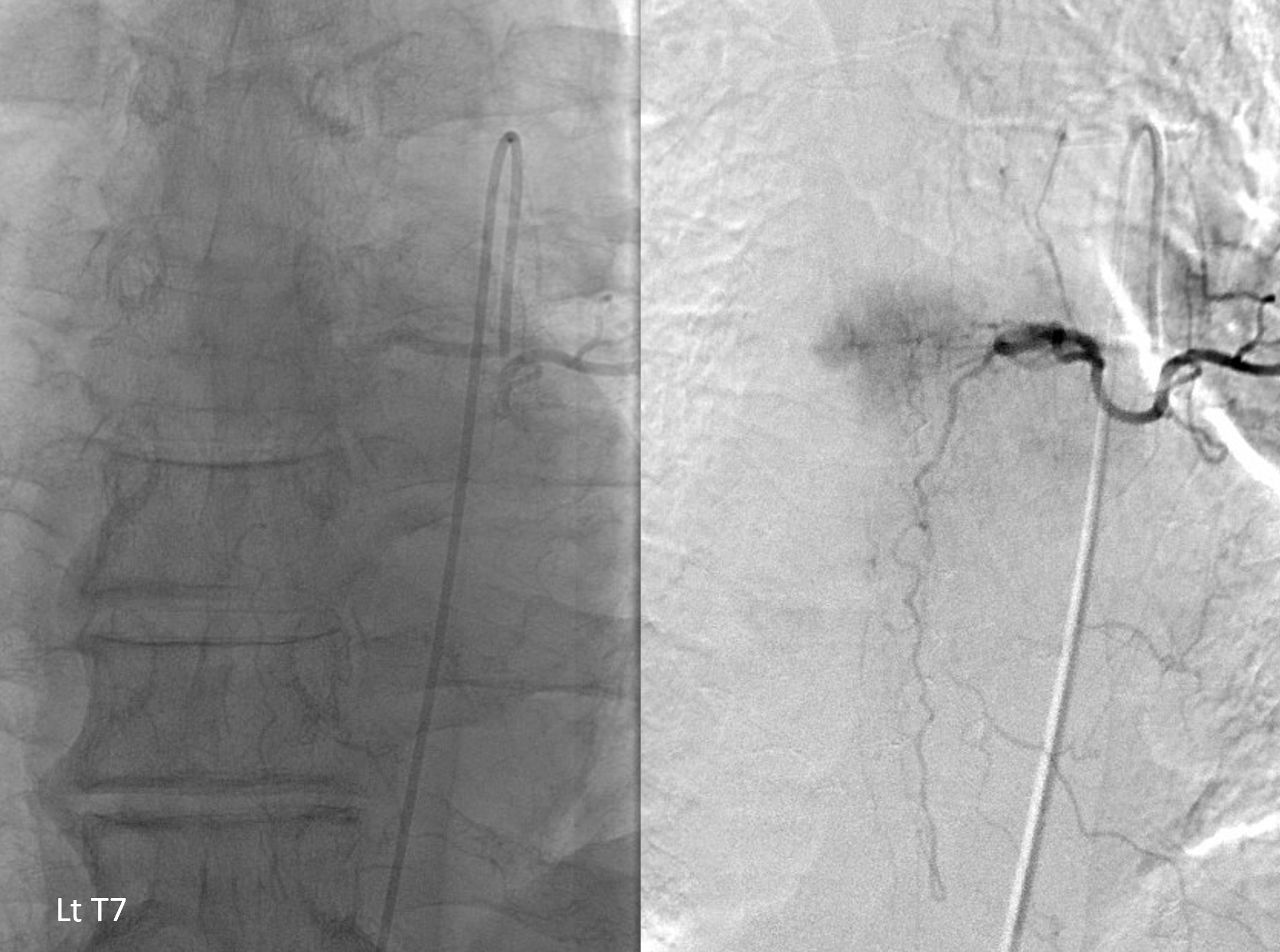
Detail view
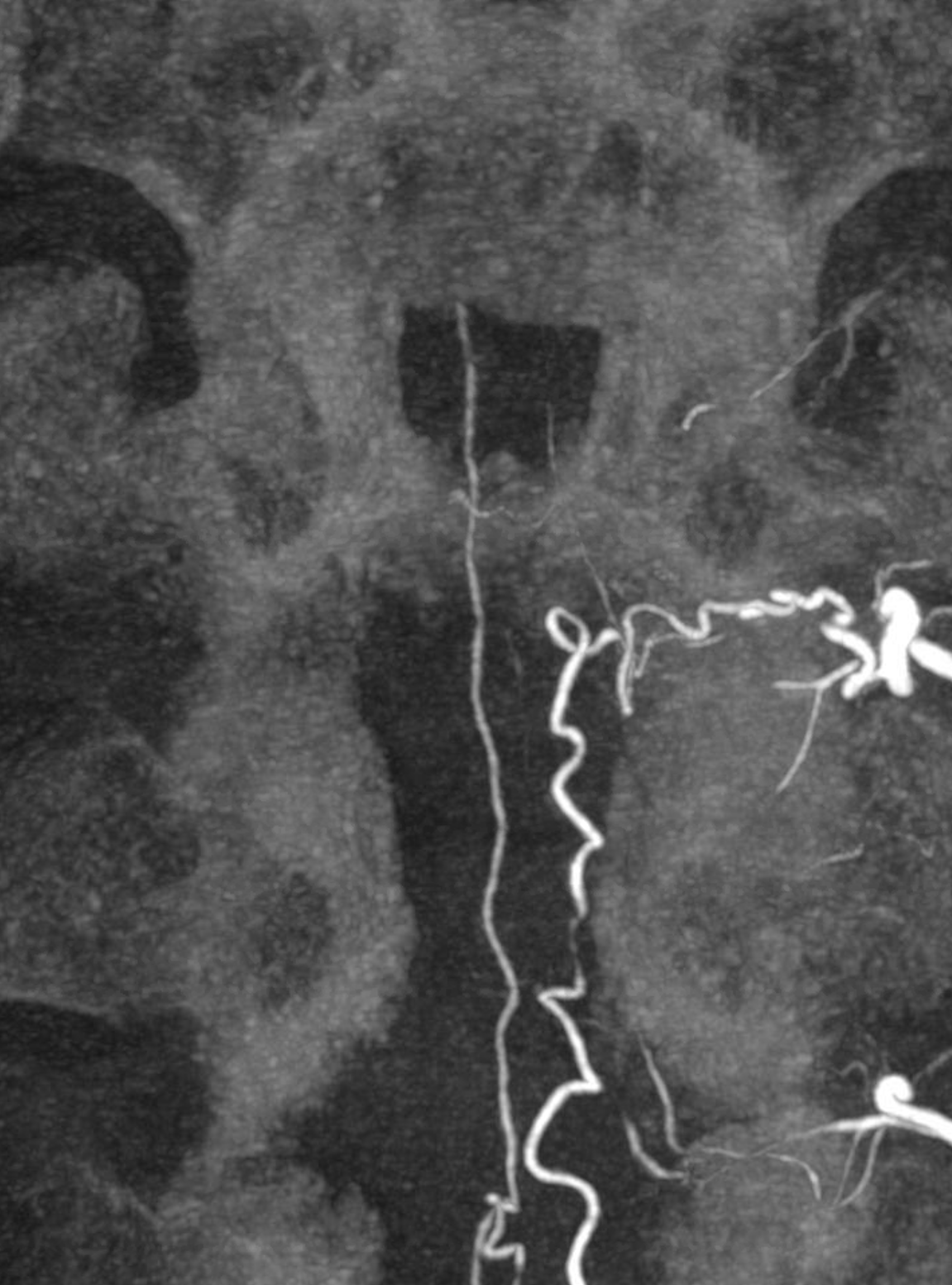
Modern spinal angiography is greatly aided by a DYNA
Shallow stereo
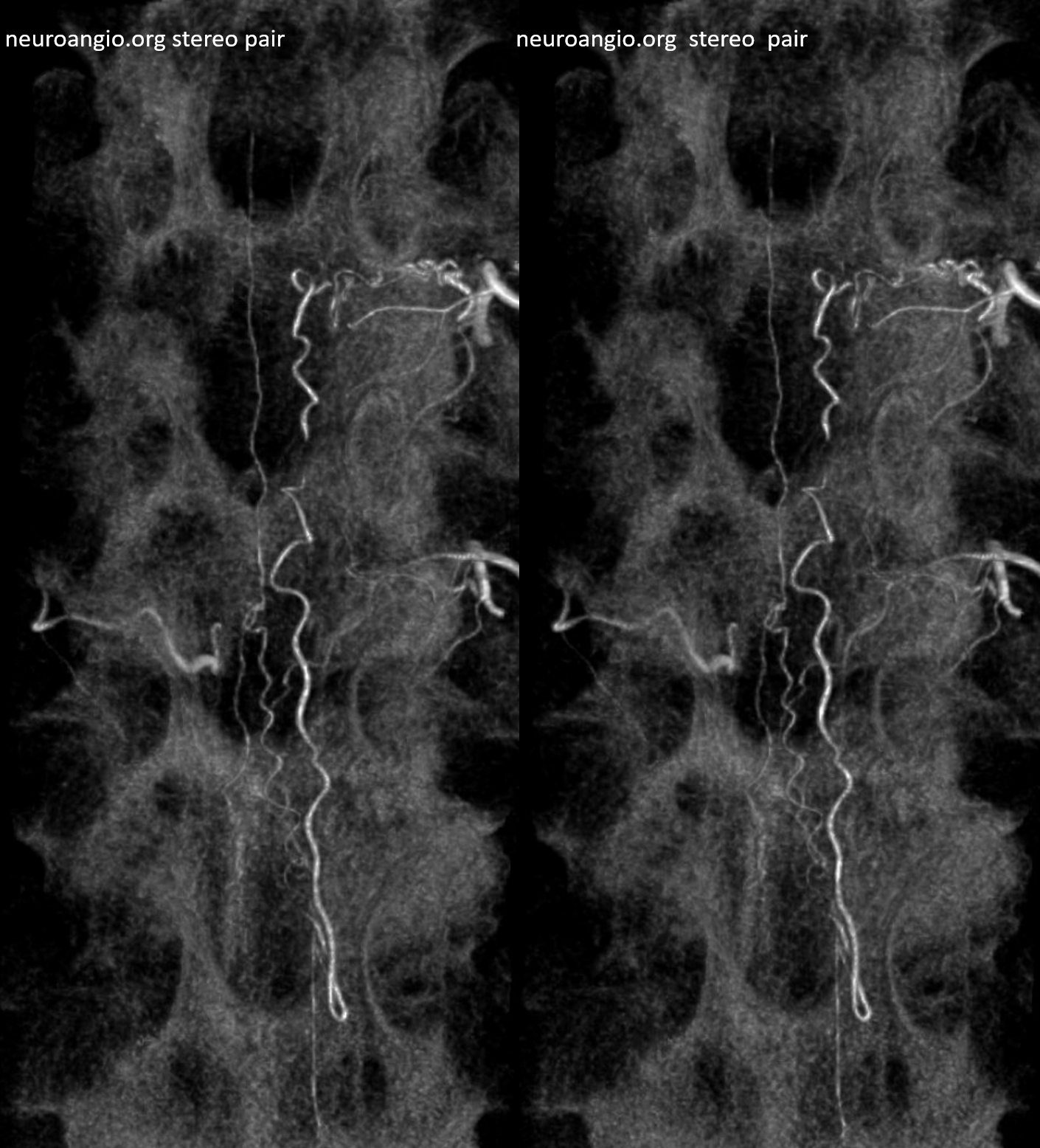
Medium depth stereo
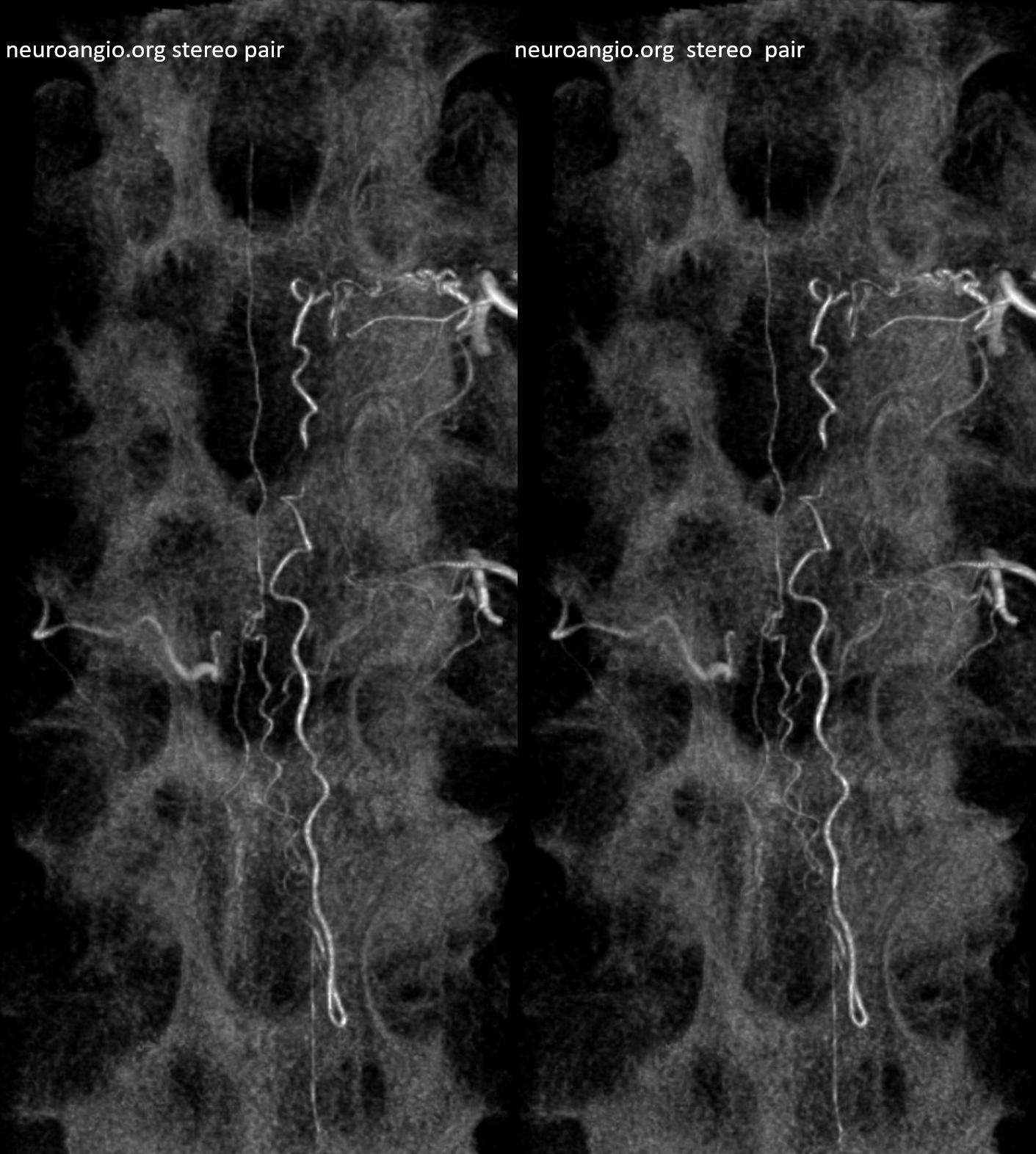
High depth stereo
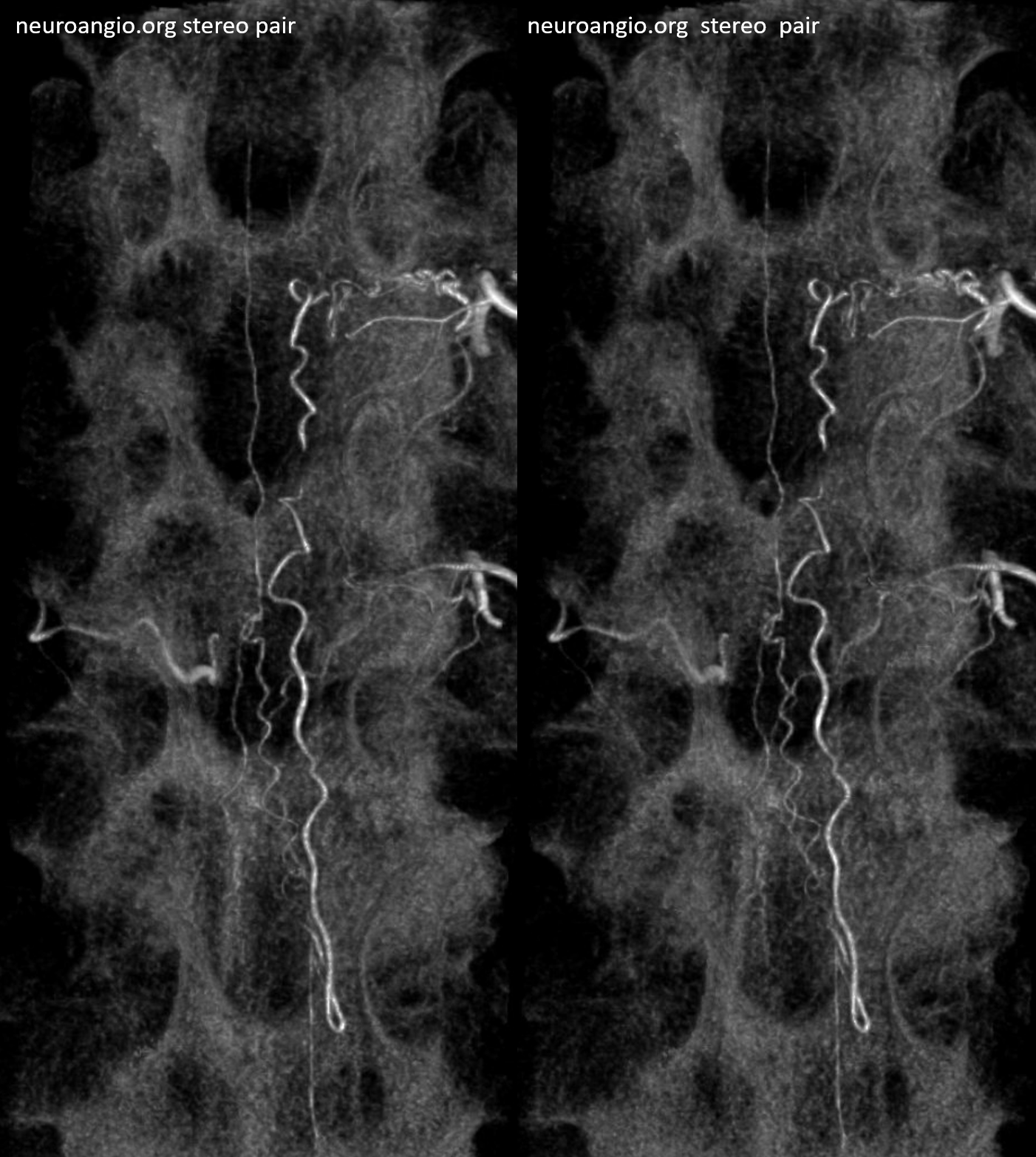
Preferred color scheme
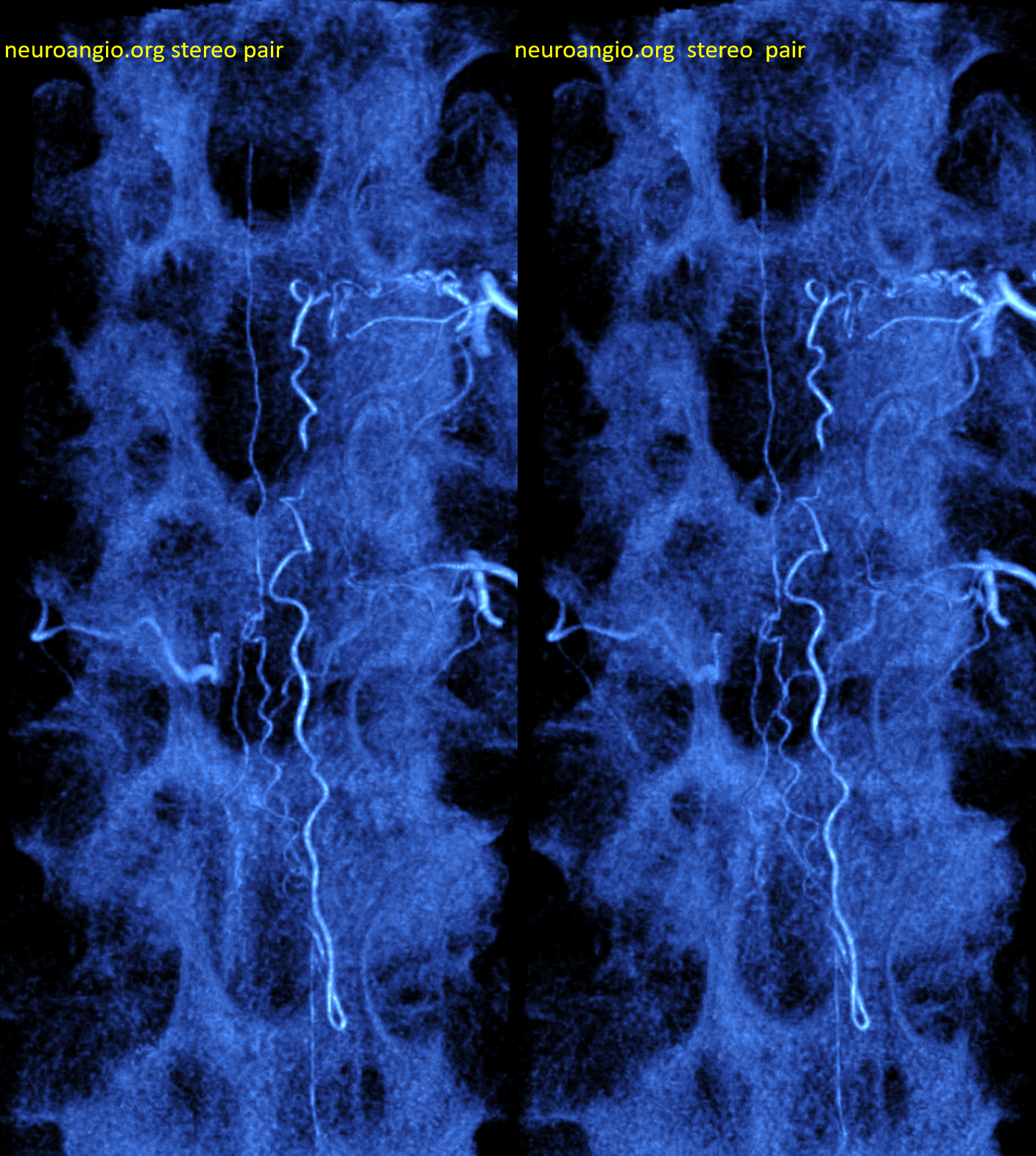
Spinal from left T9 — with no venous phase due to cord congestion. Our technique is always to identify the location of the nearby spinal supply and not stop at just finding fistula
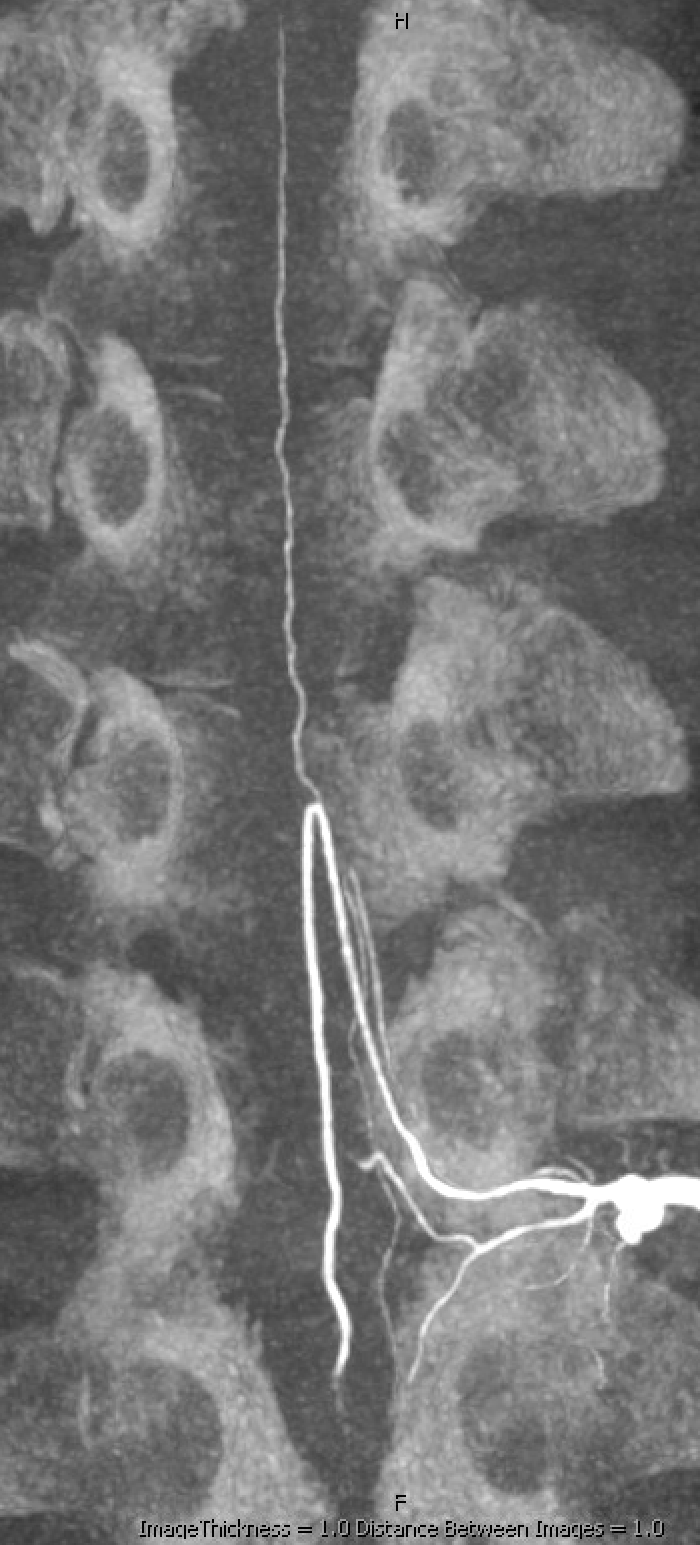
DYNA of the ASA level — check out a far larger PSA than angio here would lead us to believe. Its often like that.
Back to fistula. What the fistula level left T7 DYNA helped with a lot is understanding which branch to catheterize. This case is a perfect example of how small fistulas produce tremendous deficits. Its not about fistula size — its about degree of venous congestion. This segment of cord had no outflow and hence the big problem.
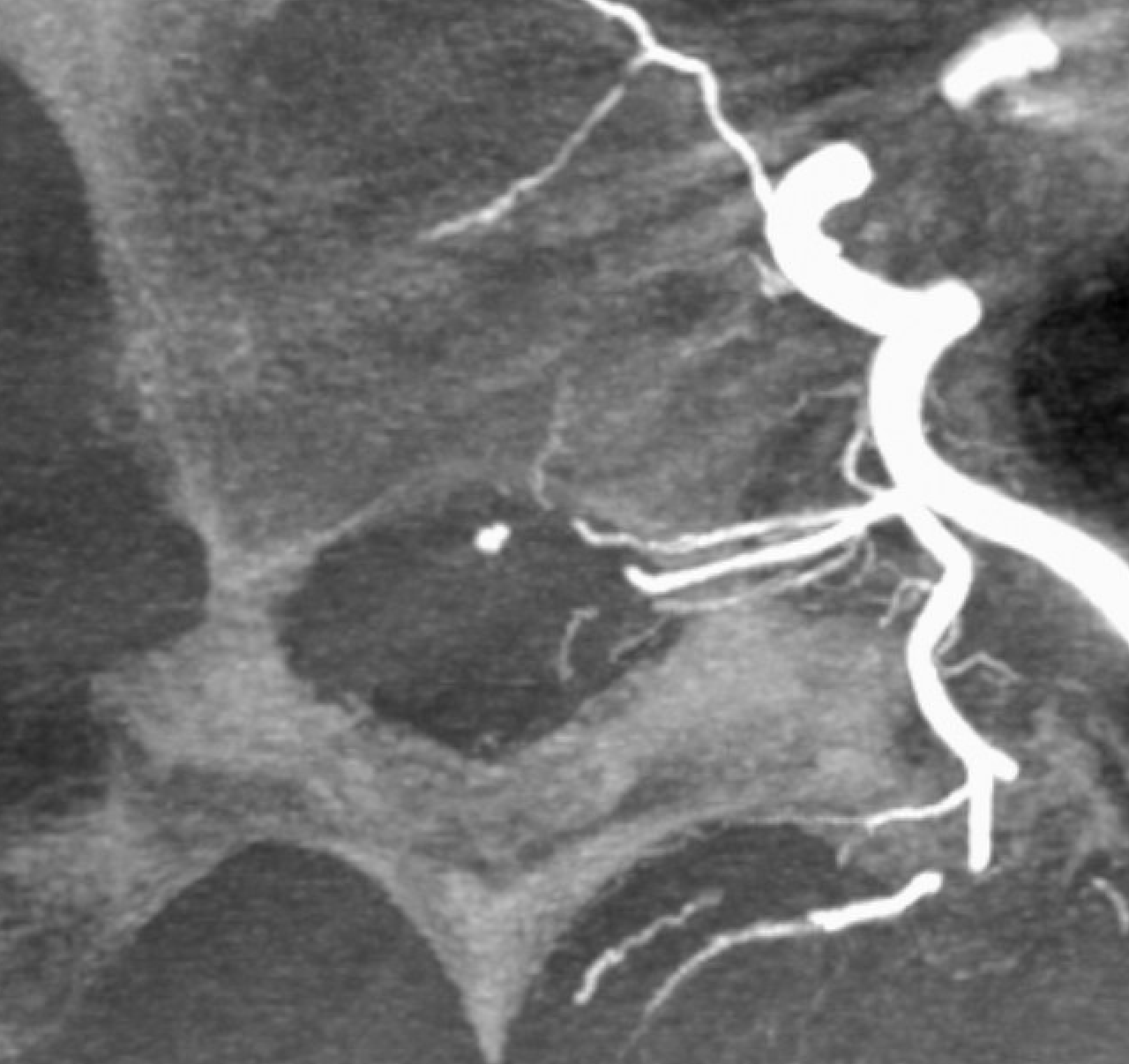
The dyna MIP below shows 3 branches — anteriormost supplies the ventral epidural arcade, middle is ventral radicular supplying fistula, and posteriormost is dorsal radicular on the dorsal T7 root.
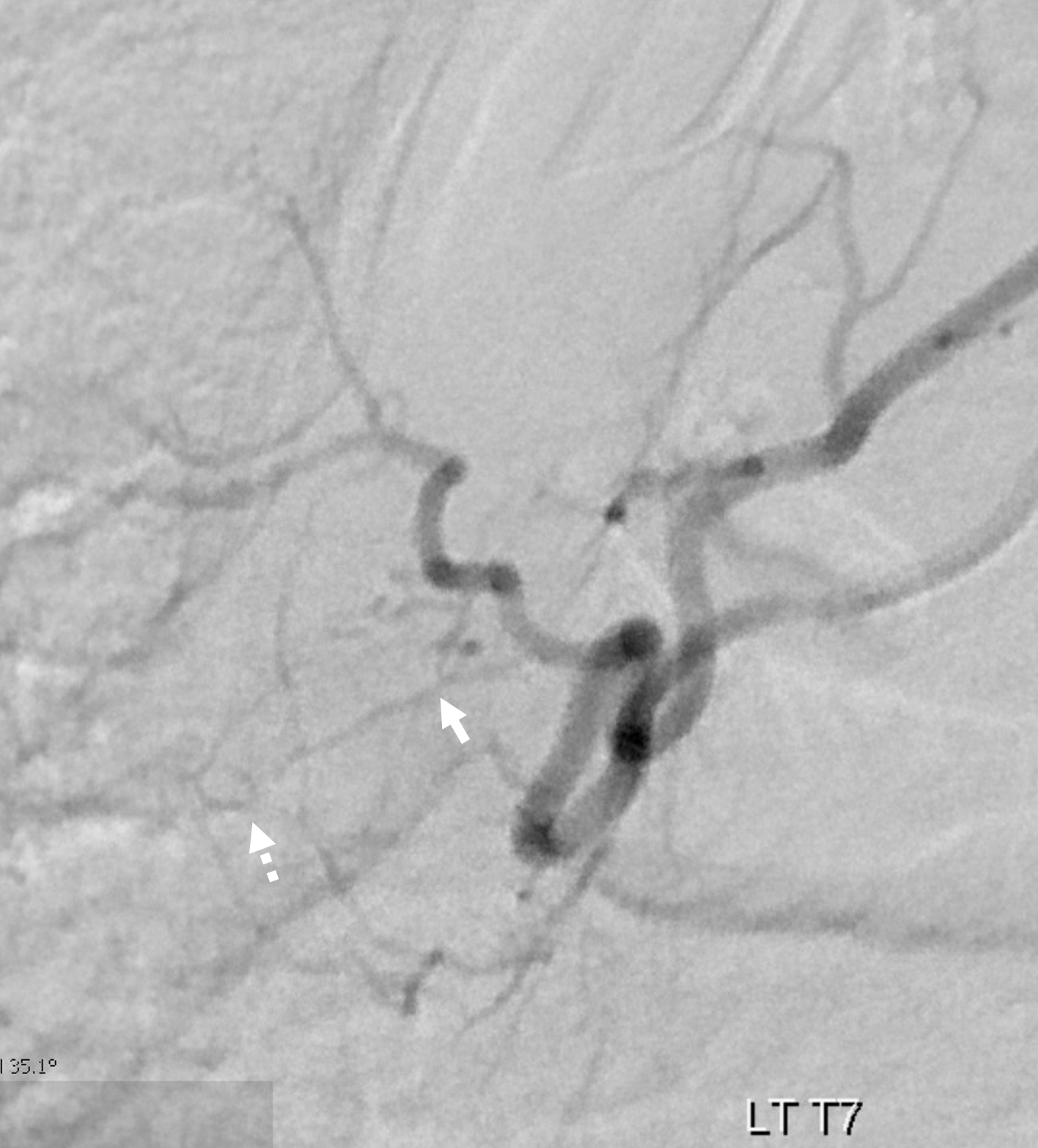
The right branch (ventral radicular artery = arrow) and fistula site is dashed arrow. Its a left cranial oblique view, determined by the DYNA
Took about 2 hours to get into it. We even coiled off the distal dorsal division in preparation for a Hail Mary Scepter C glue shot from a proximal segmental location.
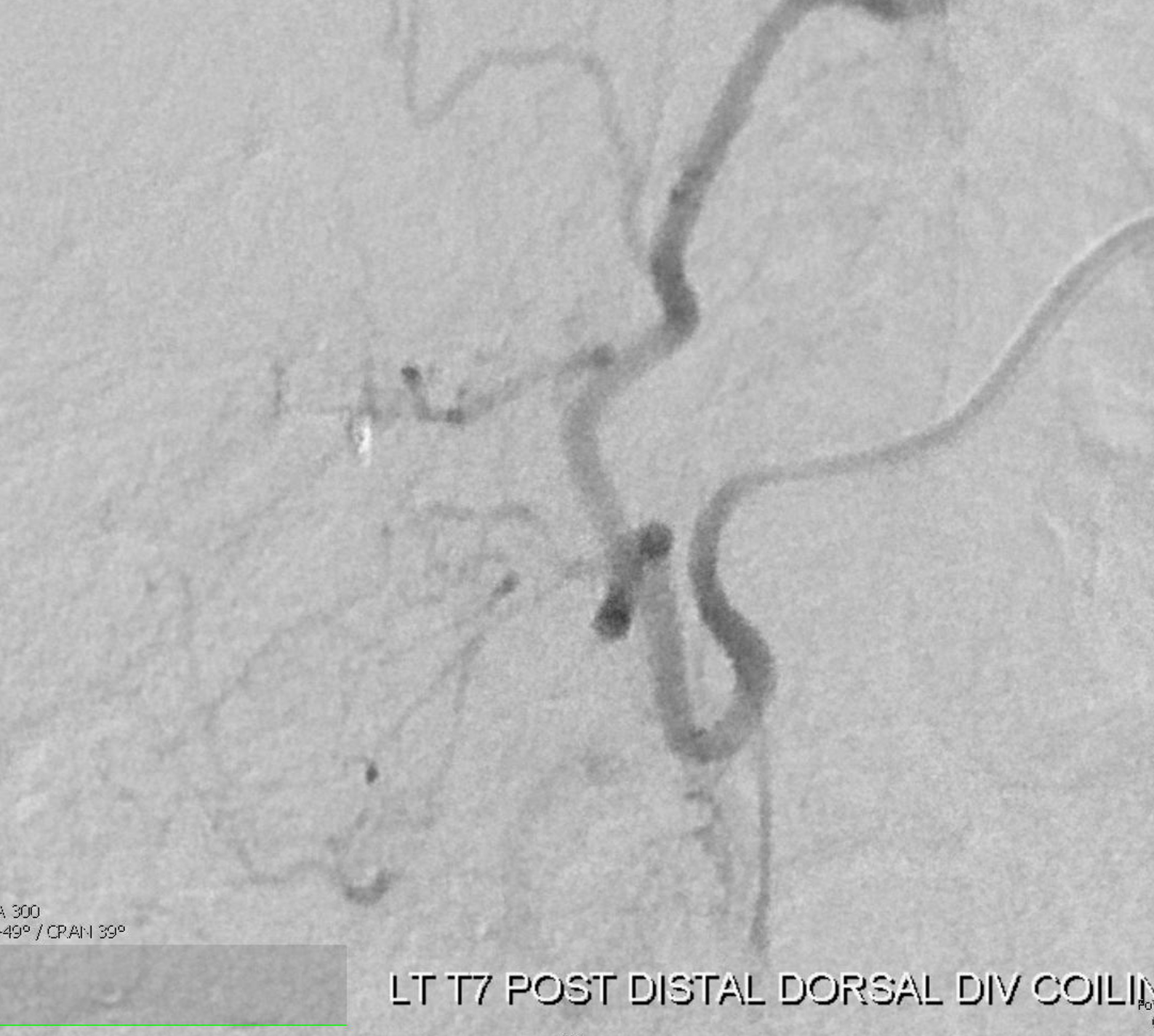
Thankfully, the combination of a Magic and Hybrid did it (tried all kinds of other things before). It was not the flow guidance that made the difference, but the smallest on market cross-section of the 1.2F Magic and its perfect marriage with the Hybrid wire
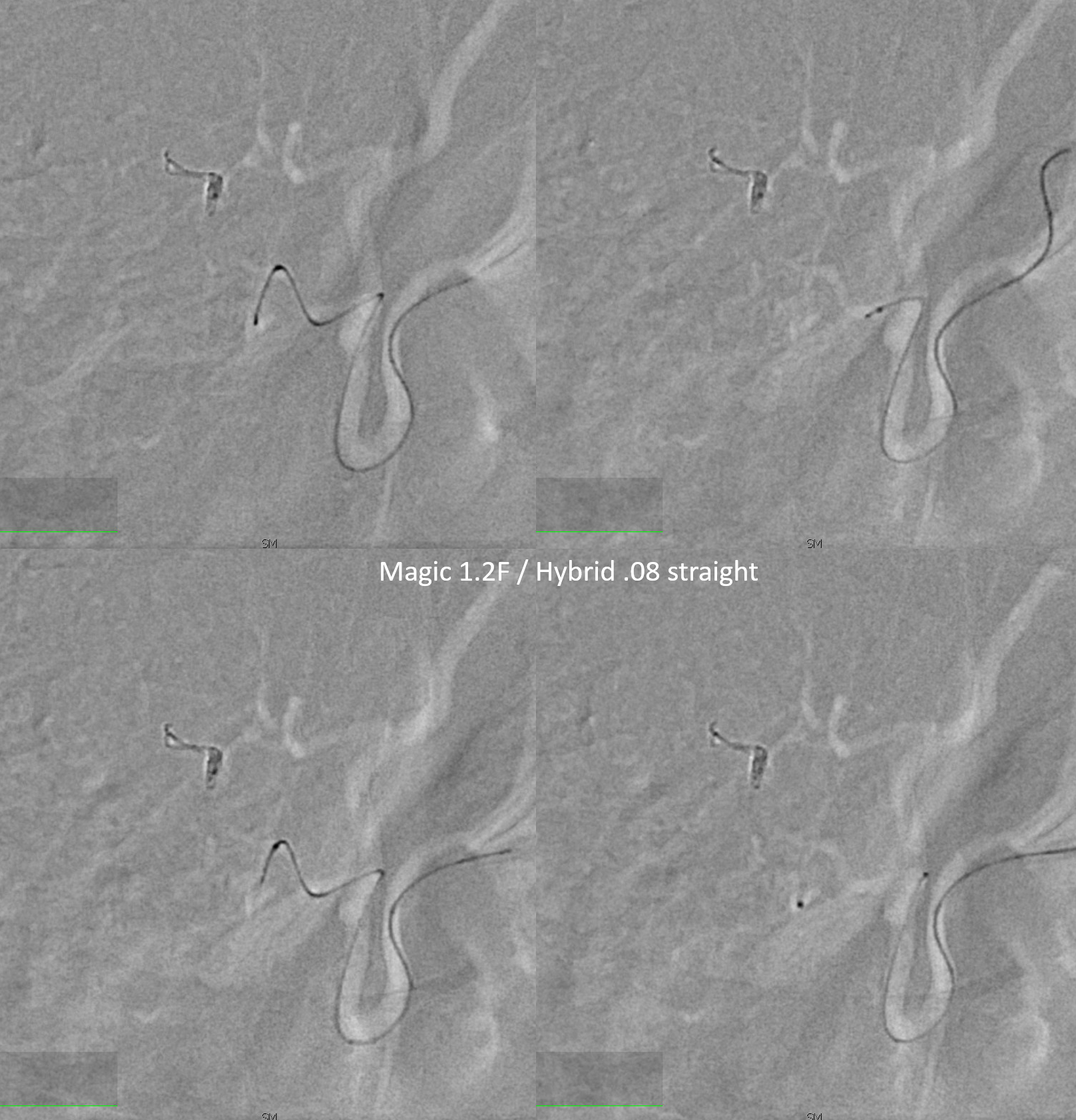
Wedge position! More good luck today!
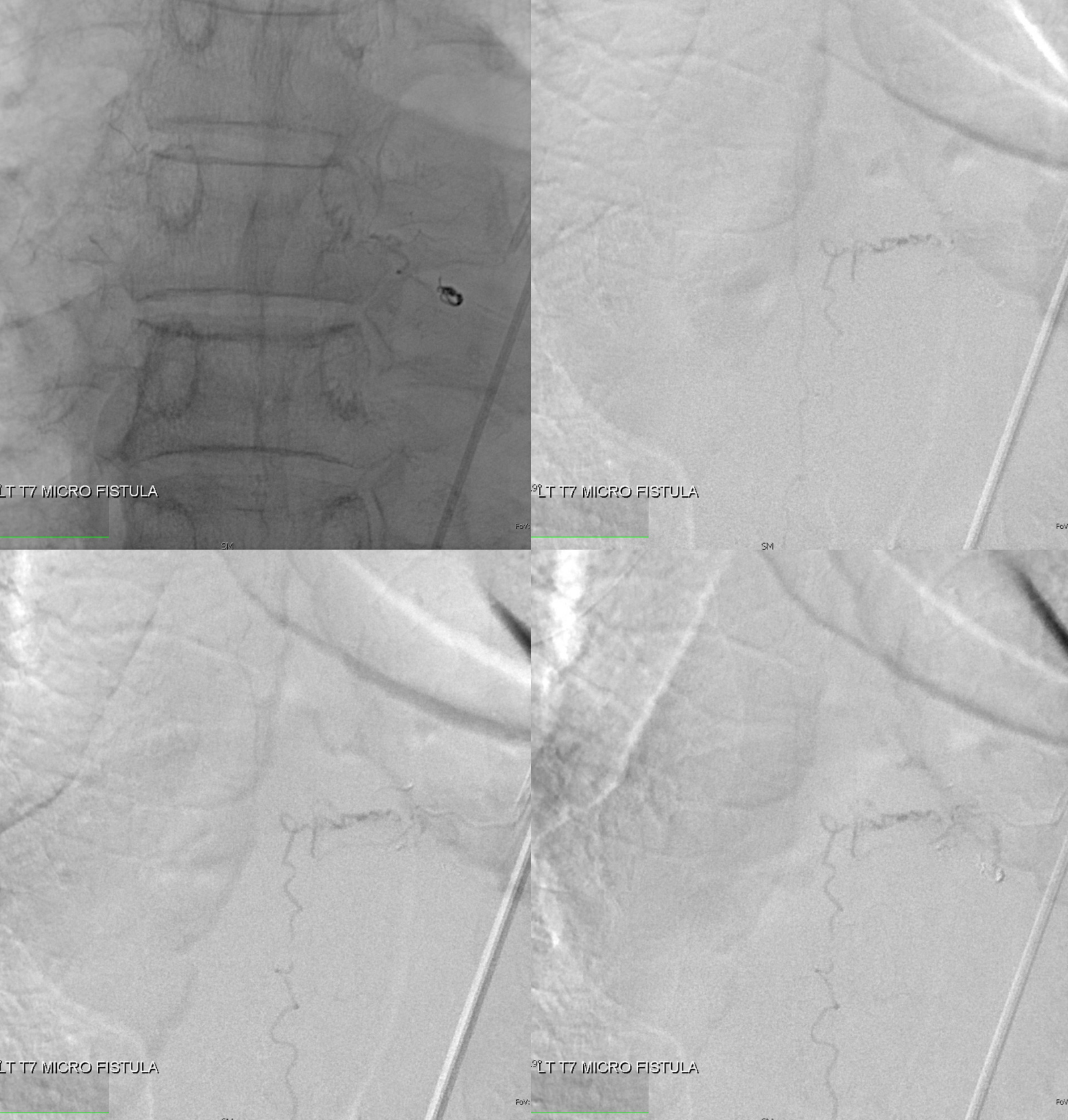
nBCA injection — worked perfectly — just at the “foot” of the vein
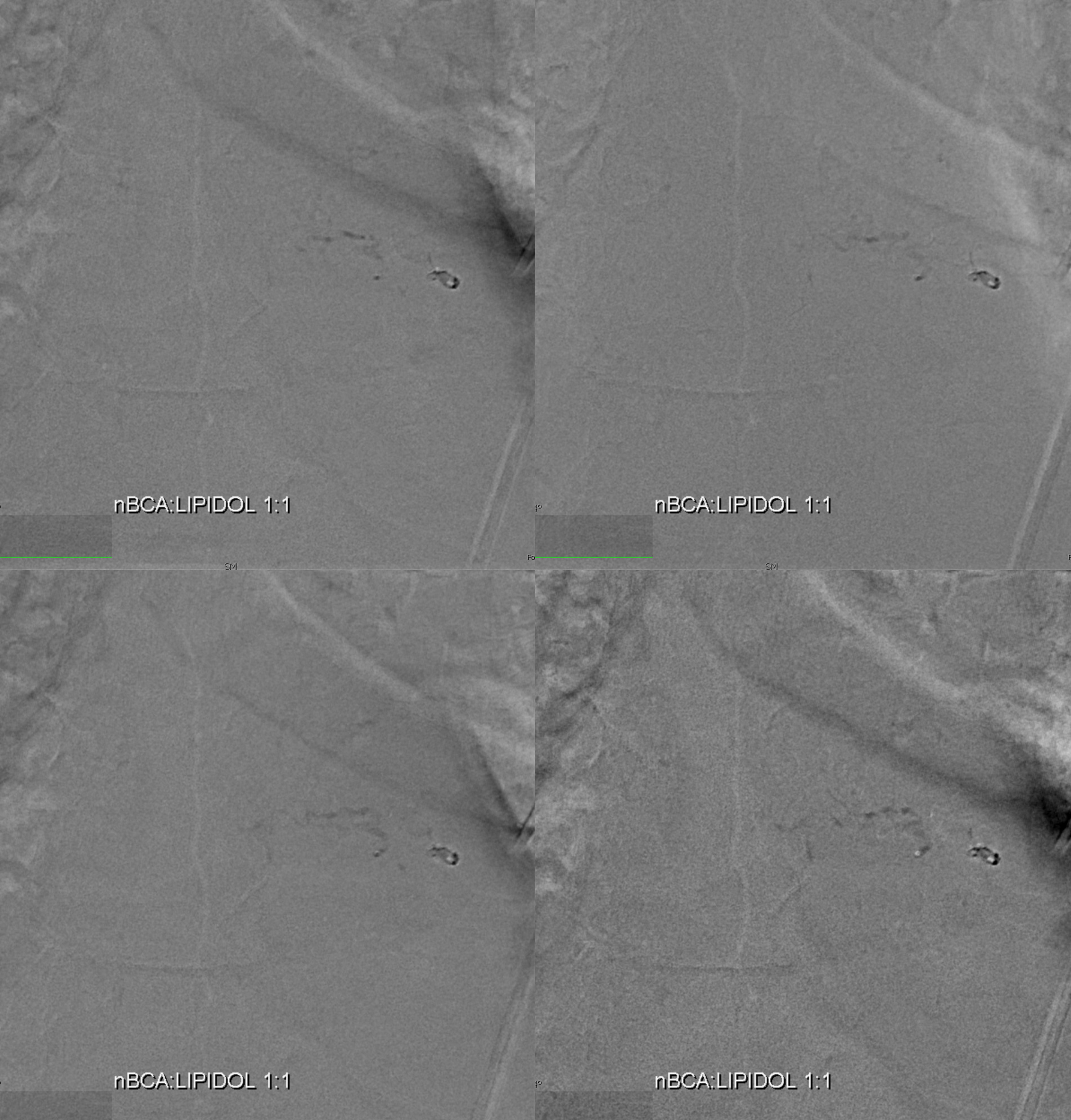
Post
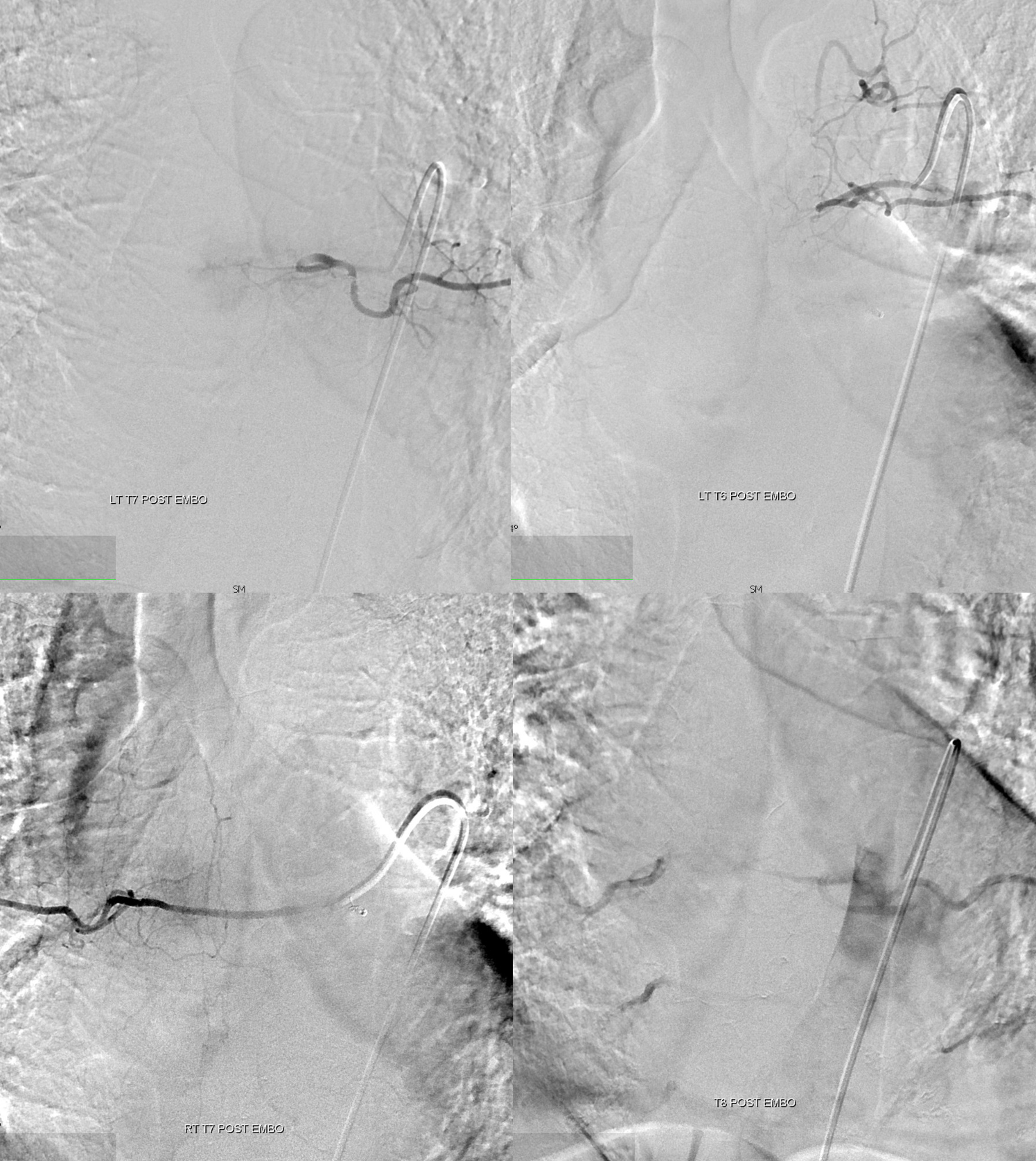
DYNA is excellent for nBCA cast — confirms foot of vein position. It is essential to have wedge control to be able to achieve this — otherwise glue is going to do something unpredictable — either not reach the fistula, or fragment and deposit in the spinal veins, or whatever — you just don’t know. With wedge flow control, it works more often than not

Now we go back to the preceding 3 angiograms. No finger pointing — just review.
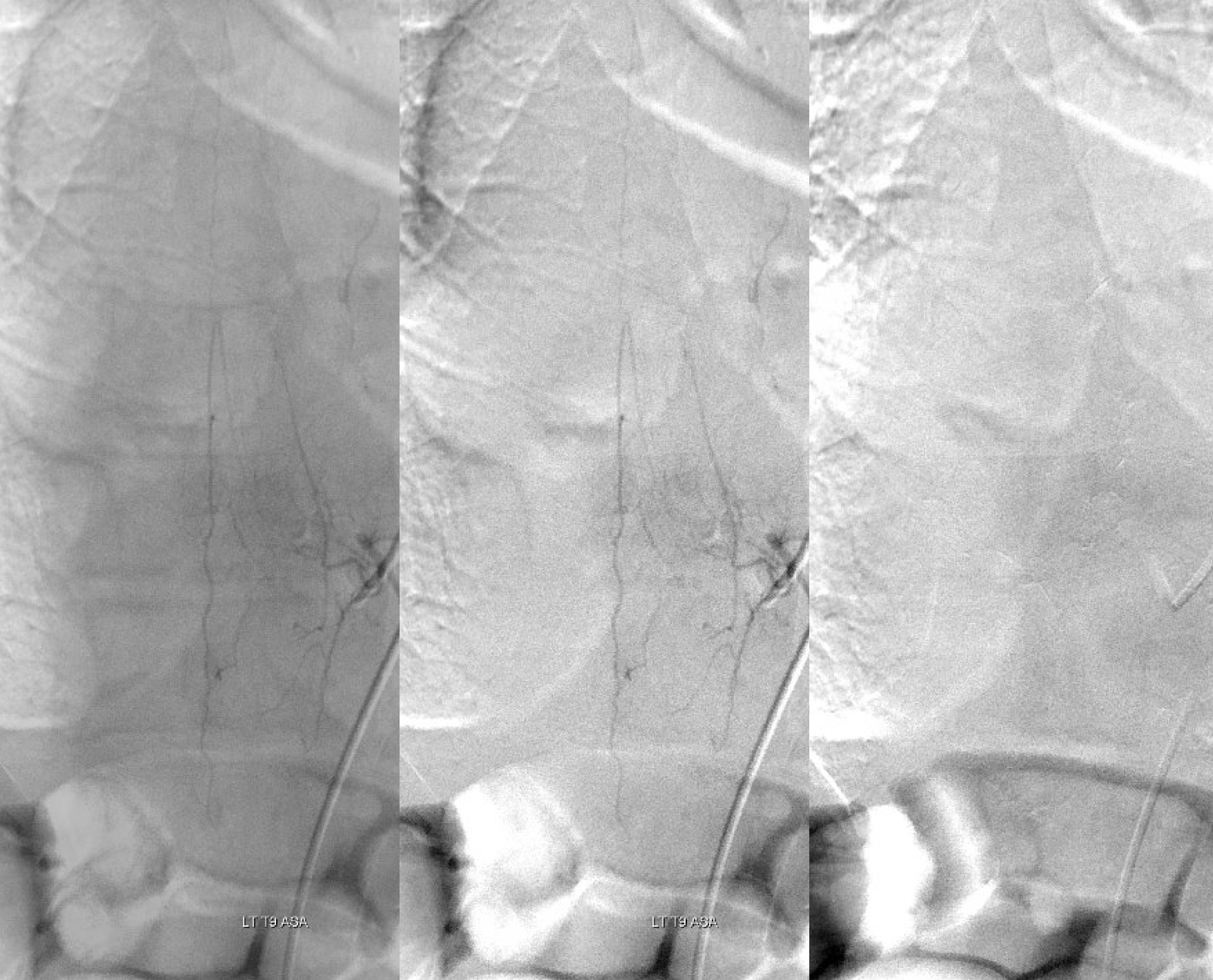
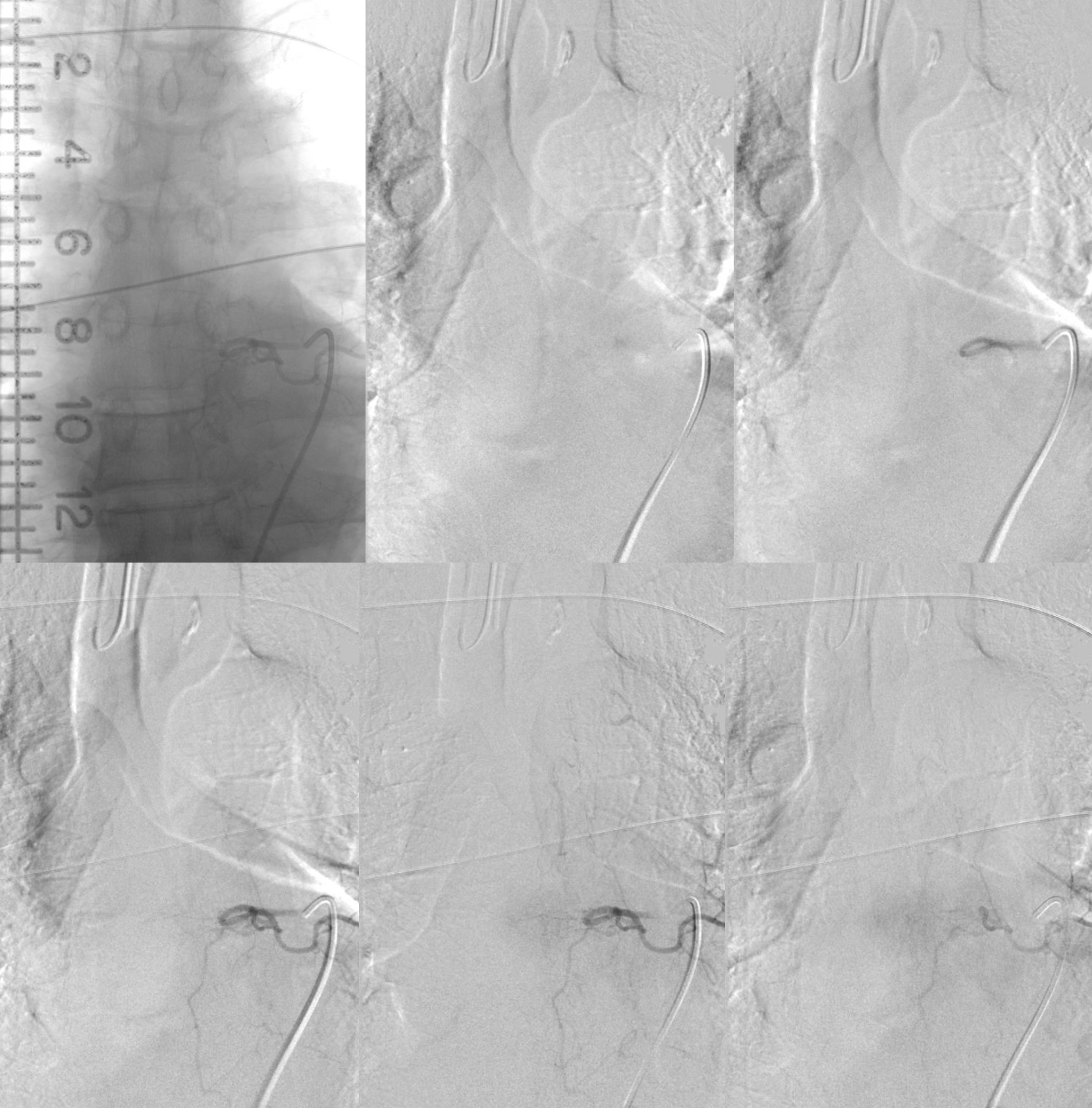
Angio 1, left T7 injection. Yes, the proximal draining vein is seen very faintly in the last, lower right frame. But it is impossible to say for sure. The problems are two — the injection is not long enough and imaging is not long enough. More contrast (about 4-6 ccs) and longer injection times would have likely picked it up. How can one tell if the injection is long enough — you should see the venous phase of the vertebral body drainage. Just like brain — need to see veins. Our frame rates for spinal are 2 fps continuous — this allows for longer imaging without too much exposure.
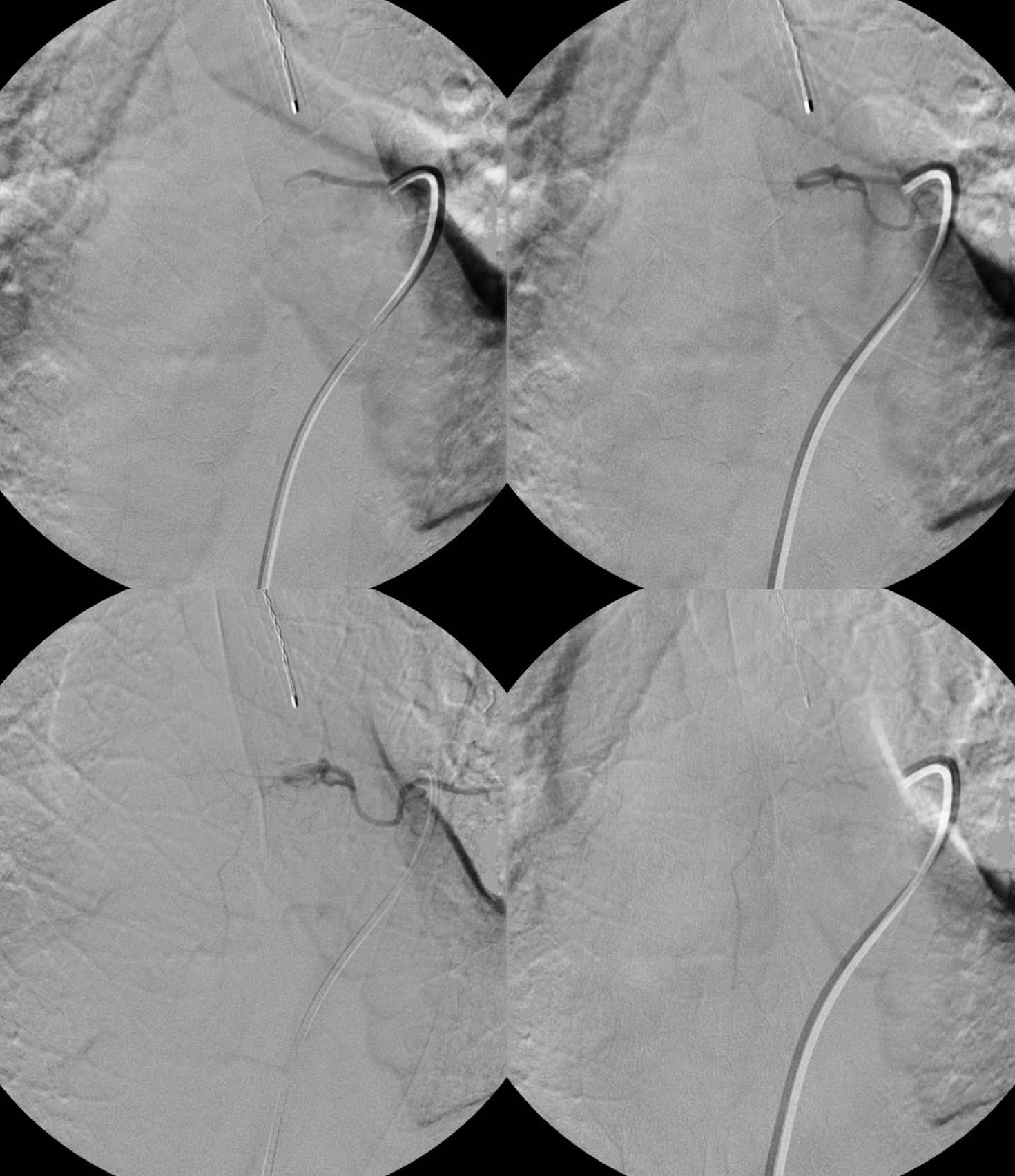
Angio 2 — here the fistula is seen, retrospectively, on multiple frames (top rightmost and all lower). The first issue is imaging window — it is not centered on the injection level, and not enough is seen below. The second issue is image review — i dont think its possible to make a definitive diagnosis here, but there is enough to go back and explore further.
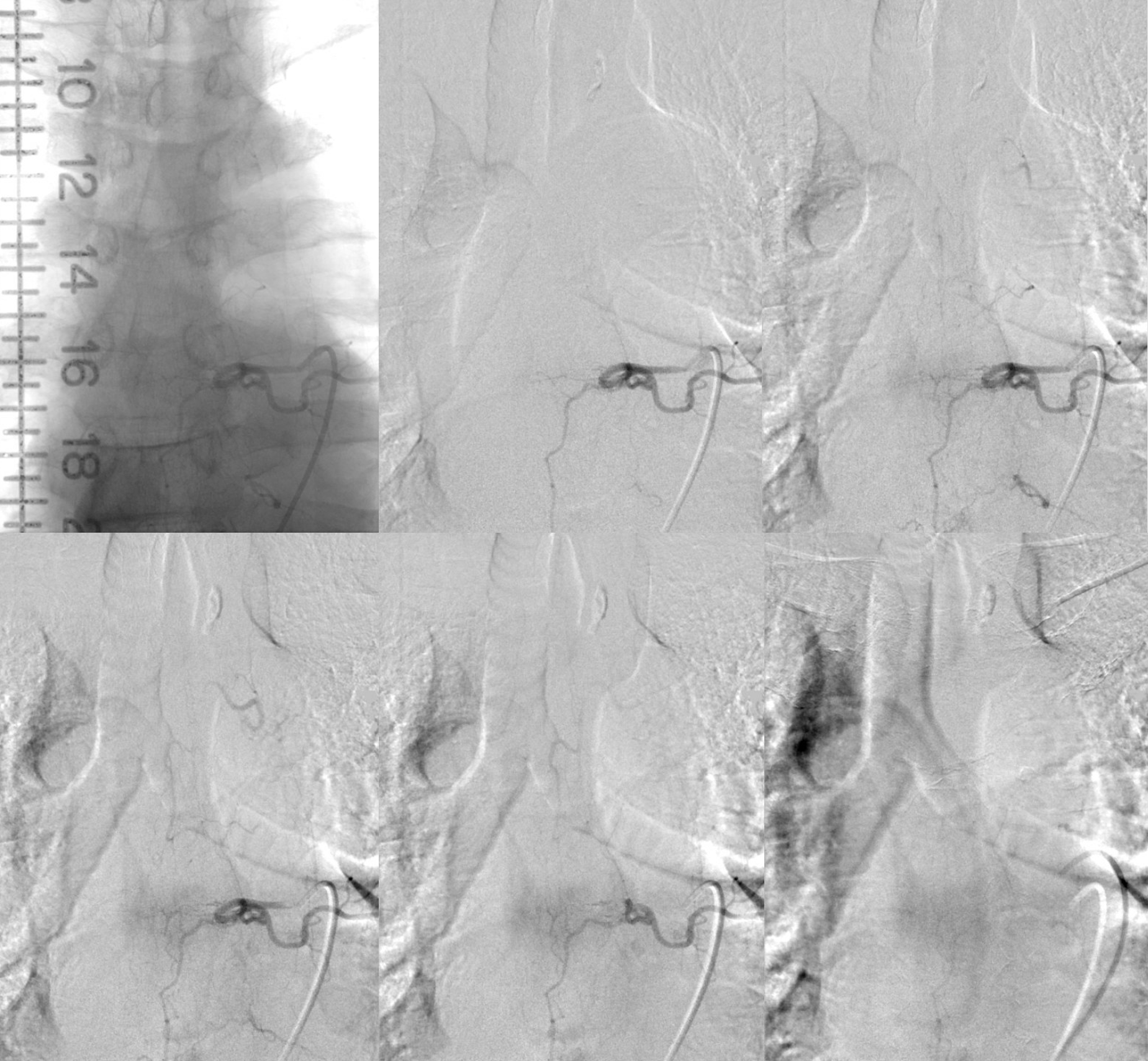
Arrows point to draining vein
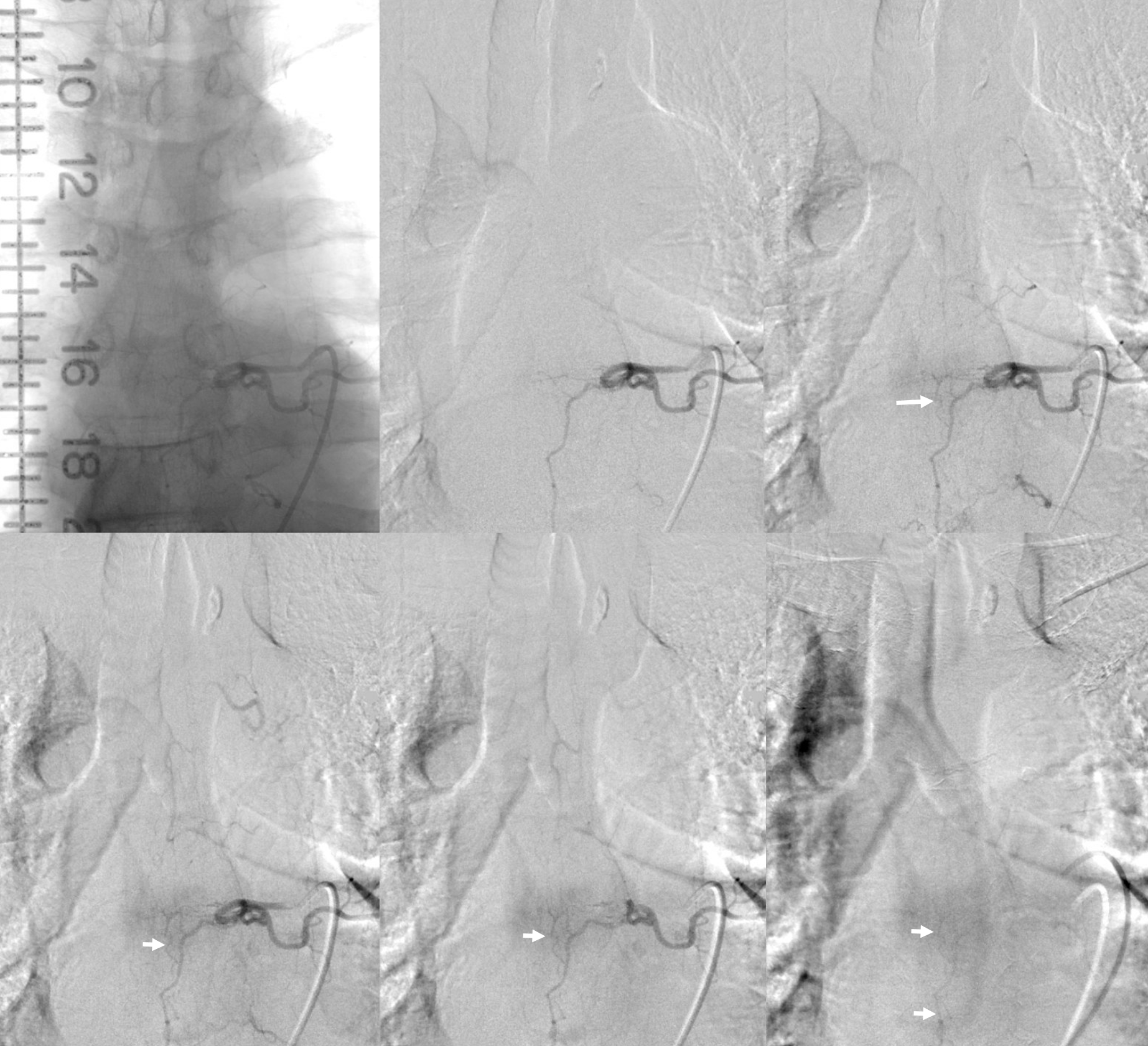
Angio 3 — Centering is better. Probably not enough contrast and not long enough imaging — see that parenchymal blush of T7 — no veins yet.
The learning points are as above. Thankfully the fistula was eventually found. This is one of a handful of repeat angios we have — in all cases, technique is the answer.
Finally, check out these anaglyphs — just for kicks
Like it? Check out other spinal dural fistula cases in Spinal Vascular Anatomy and Case Archives Sections
