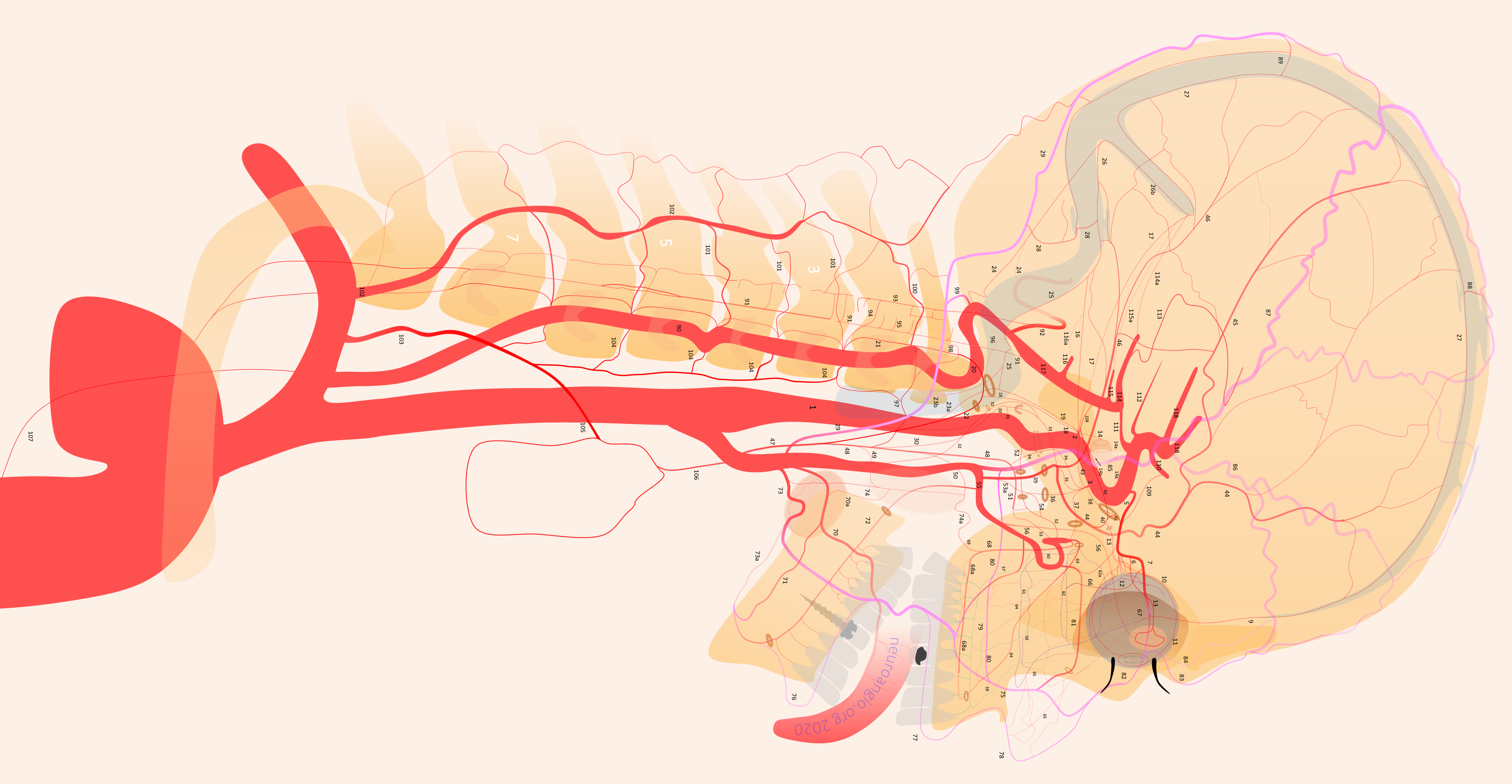
Deep Cervical Artery (102 above)
Neuroangio.org adheres to a strict vascular non-discrimination policy, which protects thyroid, ascending cervical, deep temporal, and all other “low-born” vessels. All play their part in the symphony of life — and especially in the macabre beauty of diseased life, when these ducklings can grow into brain-saving swans by reconstitution of their haughty brain-feeding neighbors.
The deep cervical artery is a branch of the subclavian artery. It runs caudocranially in the deep cervical musculature (see CTA atlas), in parallel with the vertebral artery.
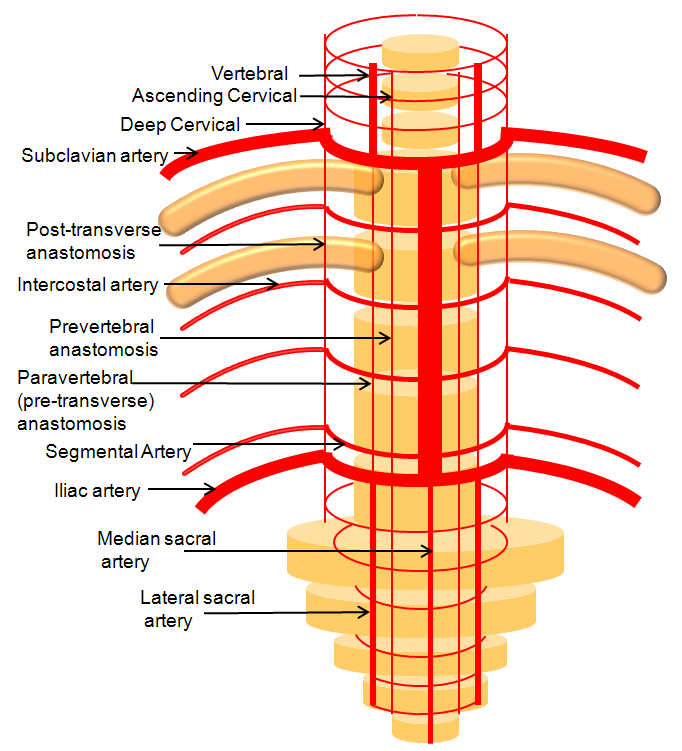
The key thing is its relationship to the vert. In the grid-like arrangement of transversely-oriented segmental arteries such as intercostal or cervical muscular arteries, the longitudinal arteries such as vert, ascending, and deep cervical vessels form a highly interconnected network. The deep cervical and vert are homologous. Occlusion of one nearly always results in reconstitution by the other. Both are connected by transversely oriented segmental muscular arteries of the C2, C3, etc levels. Below is a picture this homology, also found on the vertebral artery page

Another way to look at it is like this, highlighting homologous relationship between deep cervical artery and longitudinal anastomoses of the paraspinal arteries. See Spinal Arterial Anatomy page for additional info
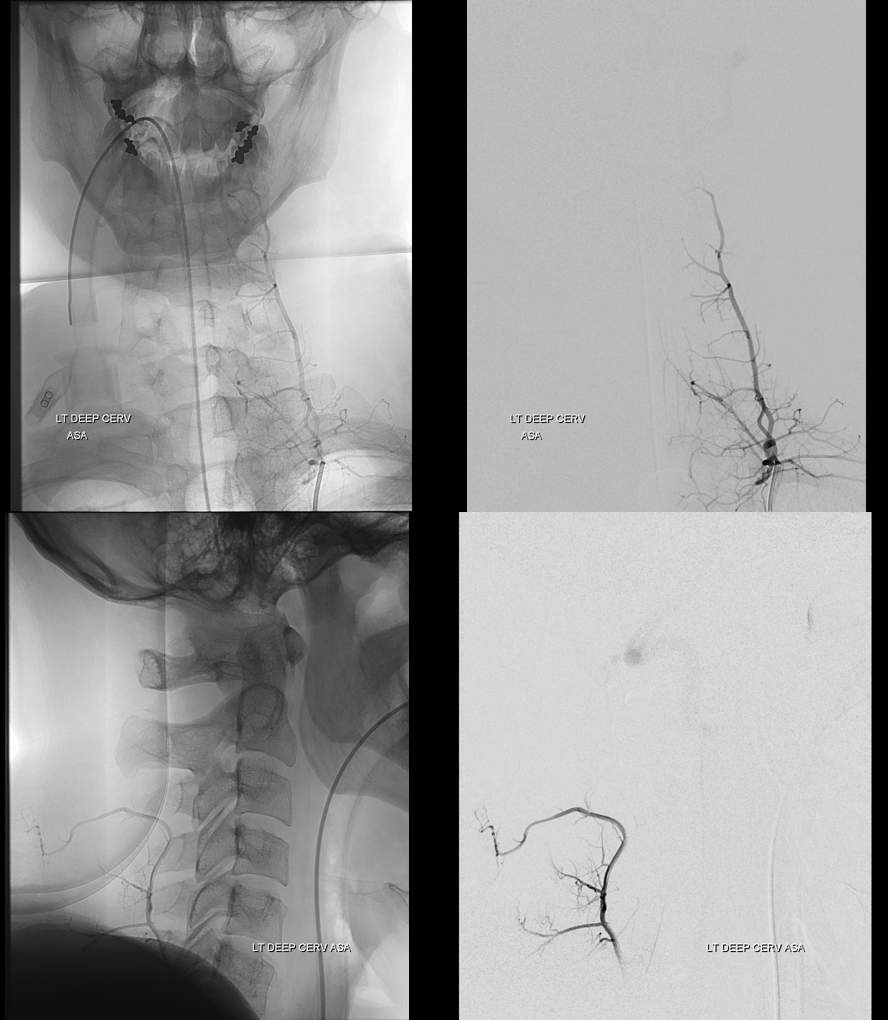
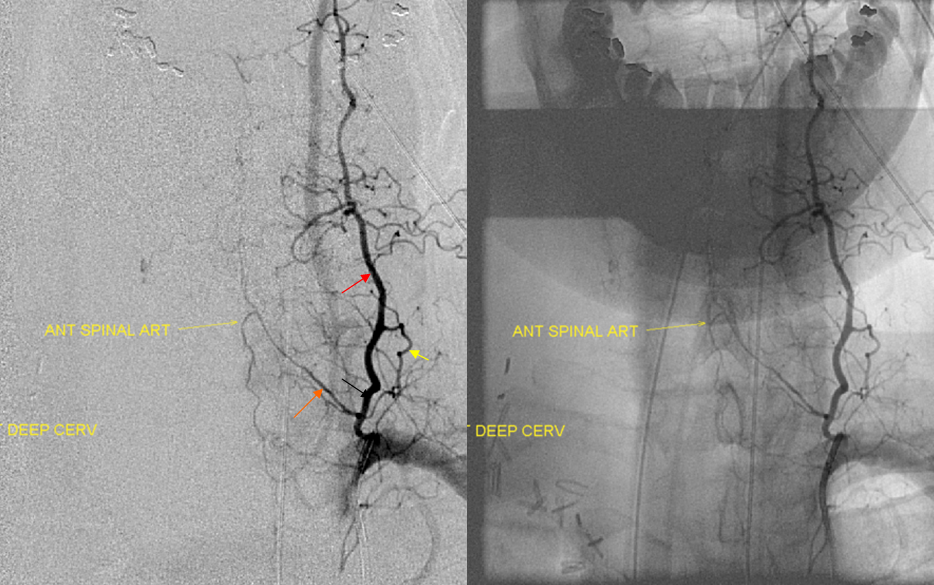
Typical angiographic view of deep cervical artery
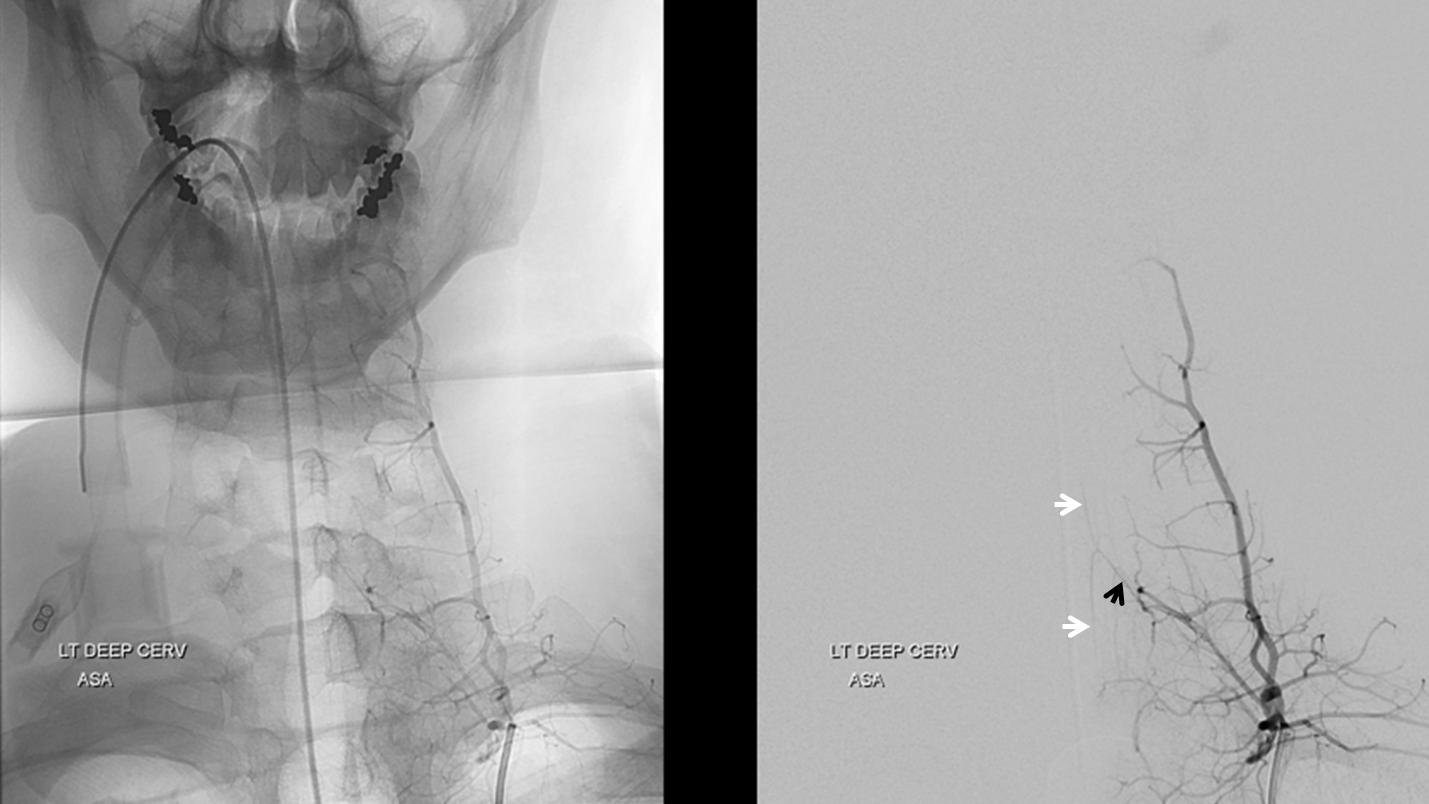
Notice supply of the anterior spinal artery (white arrows) via C7 radiculomedullary artery (black arrow). Again, in homology with the vert, deep cervical artery usually supplies the “radiculodural” arteries that vascularize the nerve roots, dura, epidural space, and (as radiculomedullary arteries) can also the spinal cord of the cervicothoracic junction. Just like vert gives rise to radiculodural and radiculomedullary arteries higher up. This can be very important, of course, when embolizing AVMs or other lesions supplied by the deep cervical artery.
Another example, with deep cervical (red) giving rise to radiculomedullary artery of C7 (orange) and anterior spinal artery
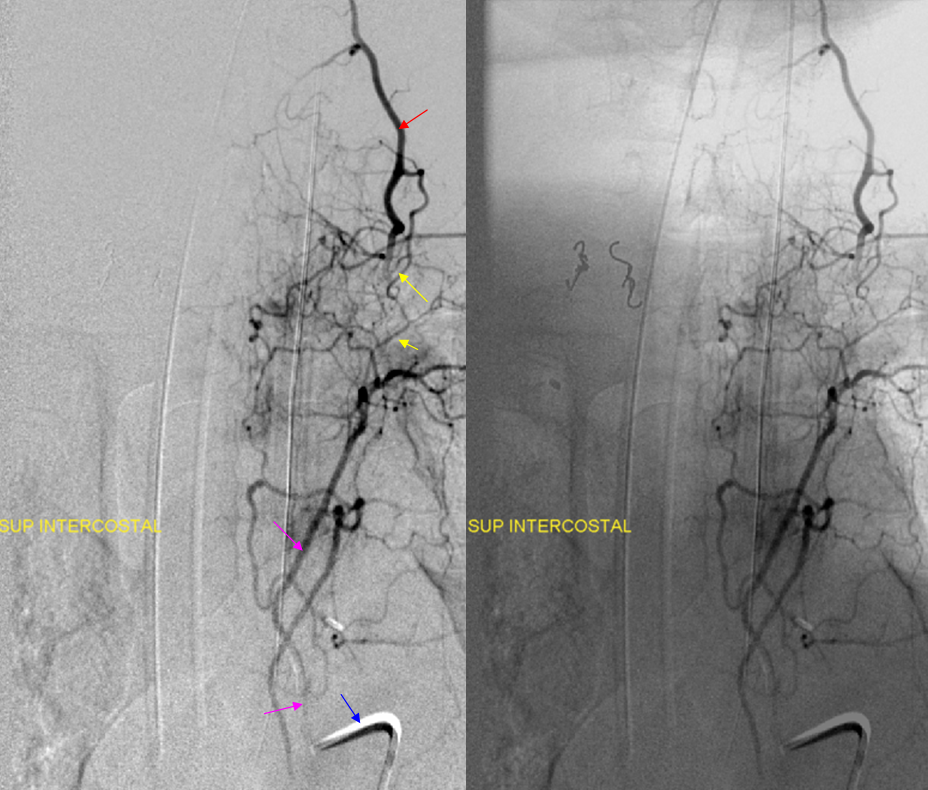
The homology of the deep cervical artery to the post-transverse anastomosis of the thoracic spinal vasculature is seen below, where the same deep cervical artery shown above is opacified by injection of the supreme intercostal artery. The supreme intercostal originates from the proximal descending aorta and supplies the vertebral elements of above the aortic arch. The supreme intercostal is, in itself, a T3 or T4 segmental artery supplying the post-transverse anastomosis, from which T1, T2, and T3 supply originates. Again, see Spinal Arterial Anatomy page for more info
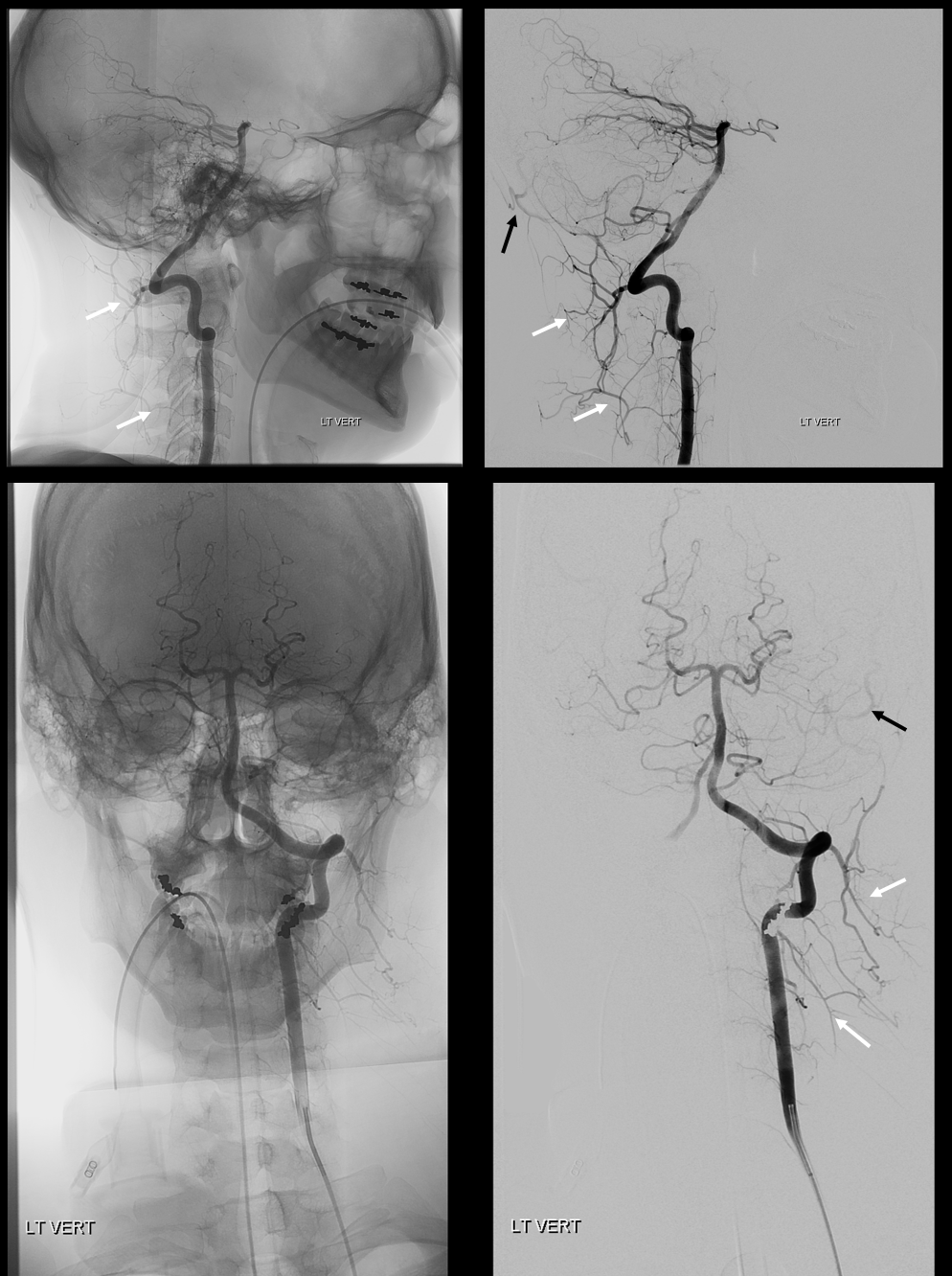
Now, both deep cervical and vert share supply of cervical musculature via those segmental muscular arteries. Like in everything else, there is balance. Sometimes, deep cervical is the dominant vessel feeding those neck muscles, sometimes vert, sometimes both. Here is an example of vert dominance via segmental muscular branches (white). Notice flash filling of the occipital artery (black). For more of that see occipital artery page
Stereo views
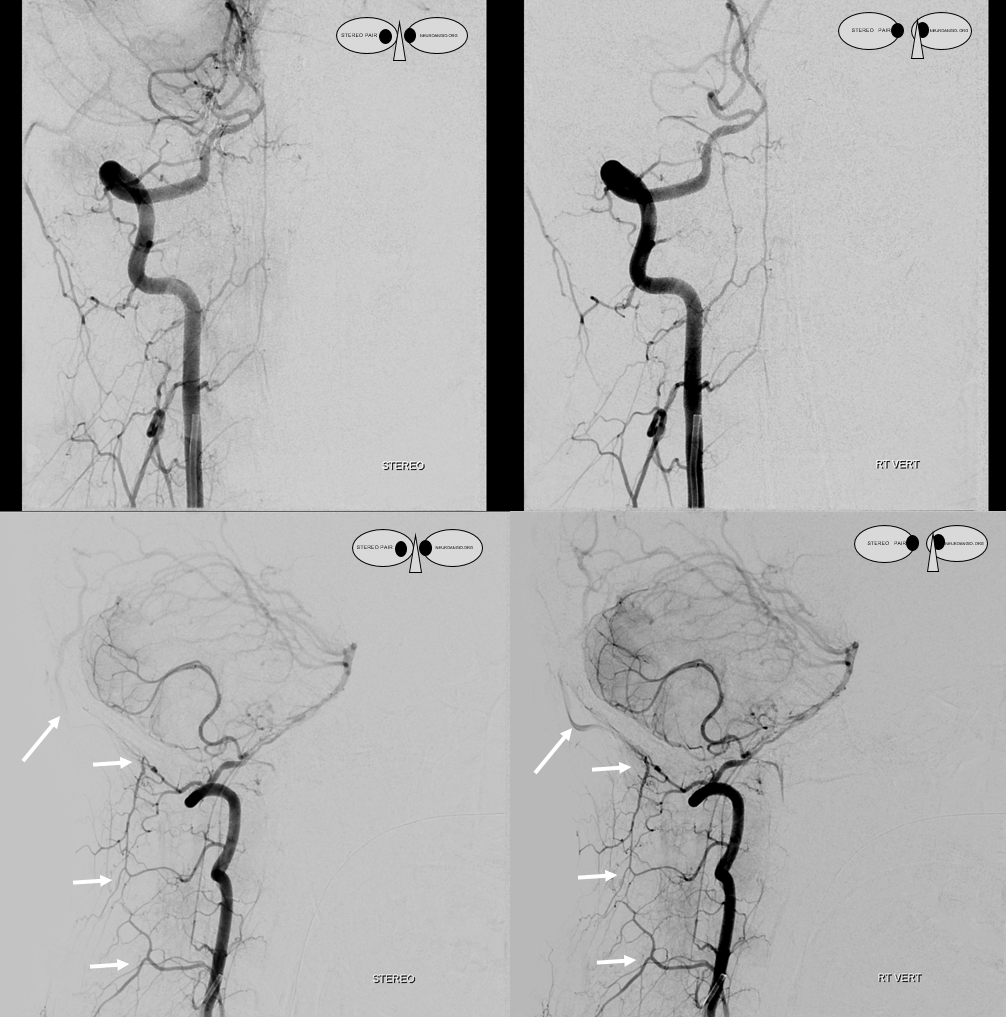
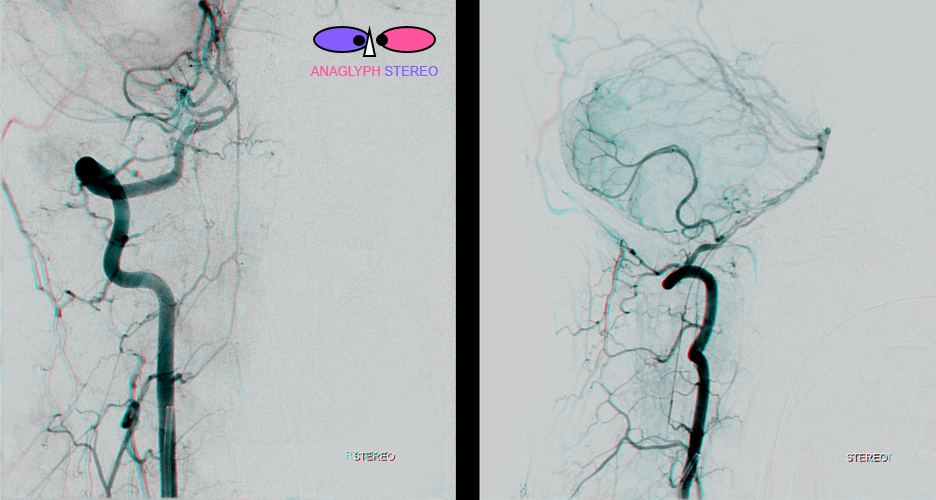
Native anaglyph stereo
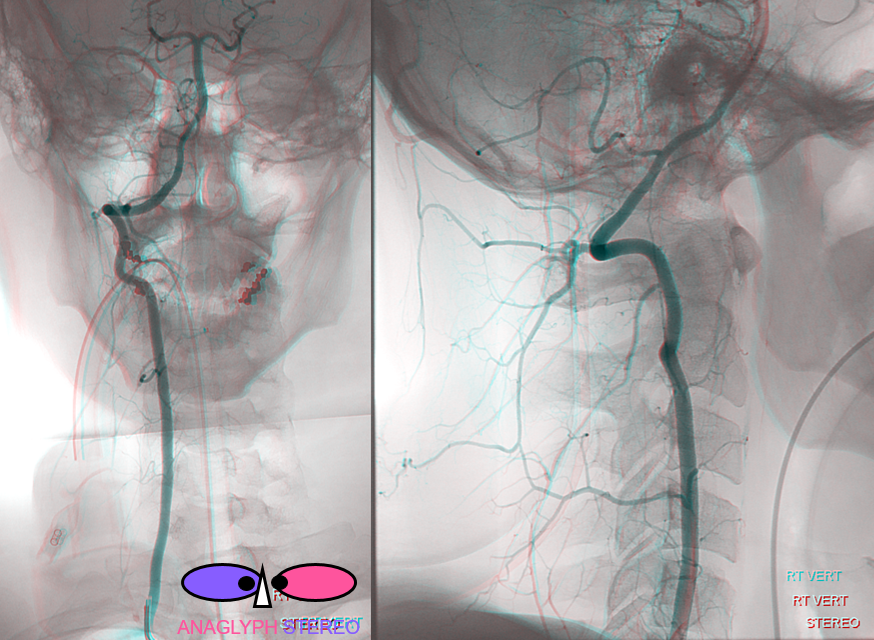
Yet another example of hypoplastic deep cervical artery (yellow) with its distal territory taken over by the vert via C3 muscular branch (red)
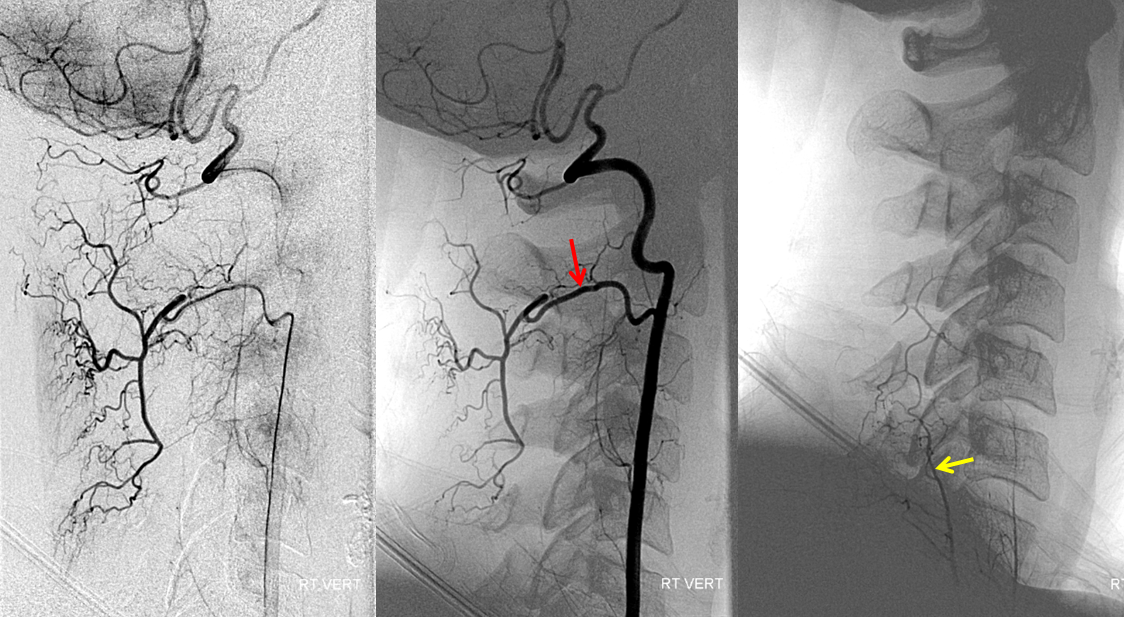
A beautiful example of vertebral injection, connecting to all 4 longitudinal axes (deep cervical, ascending cervical, vertebral, and anterior spinal) via multiple transverse muscular segmental arteries
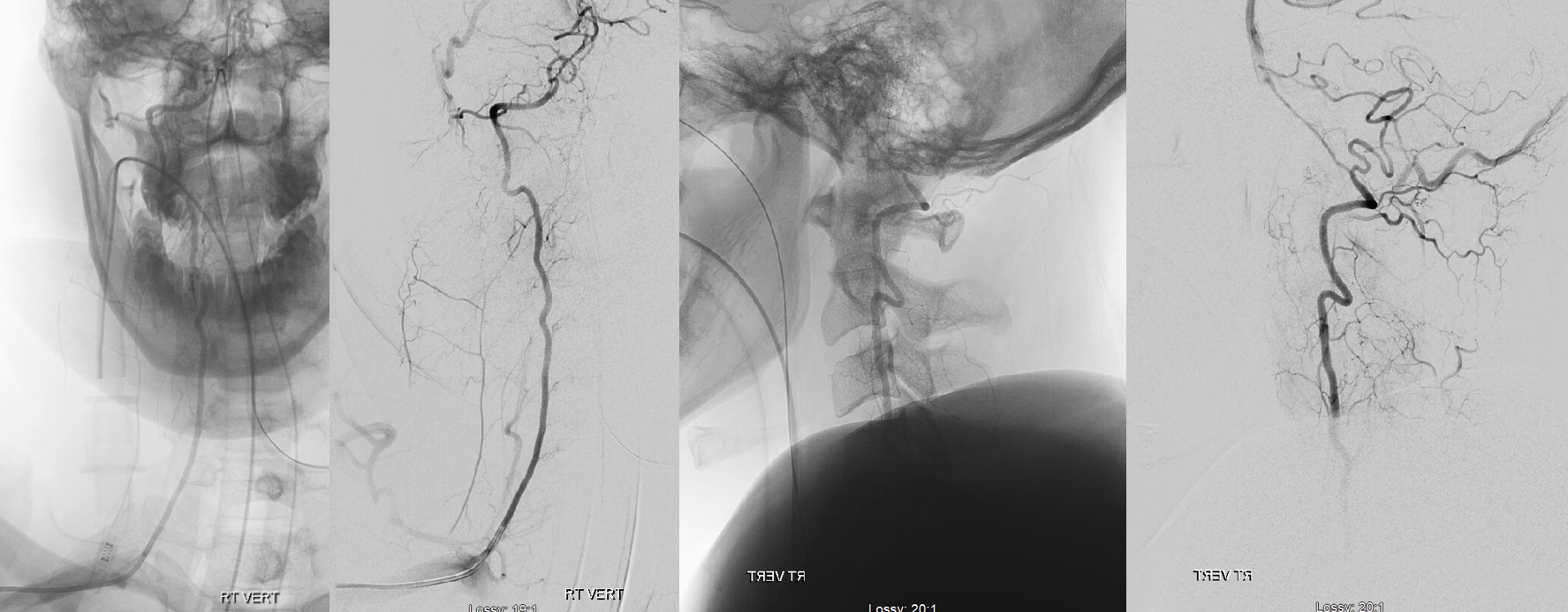

Hemodynamic Factors
Much of what you see above for these and all kinds of connections in general is influenced by hemodynamics. The pressure of injection can and often does change flow direction, patterns, etc. For example, in images below, during active contrast injection, the injection pressure in right vertebral artery exceeds arterial pressure, reversing flow in muscular anastomoses to both transiently opacify the deep cervical artery (arrows) and reverse flow in the left vert (dashed arrow). When injection is done (right images), the deep cervical is not longer visualized.
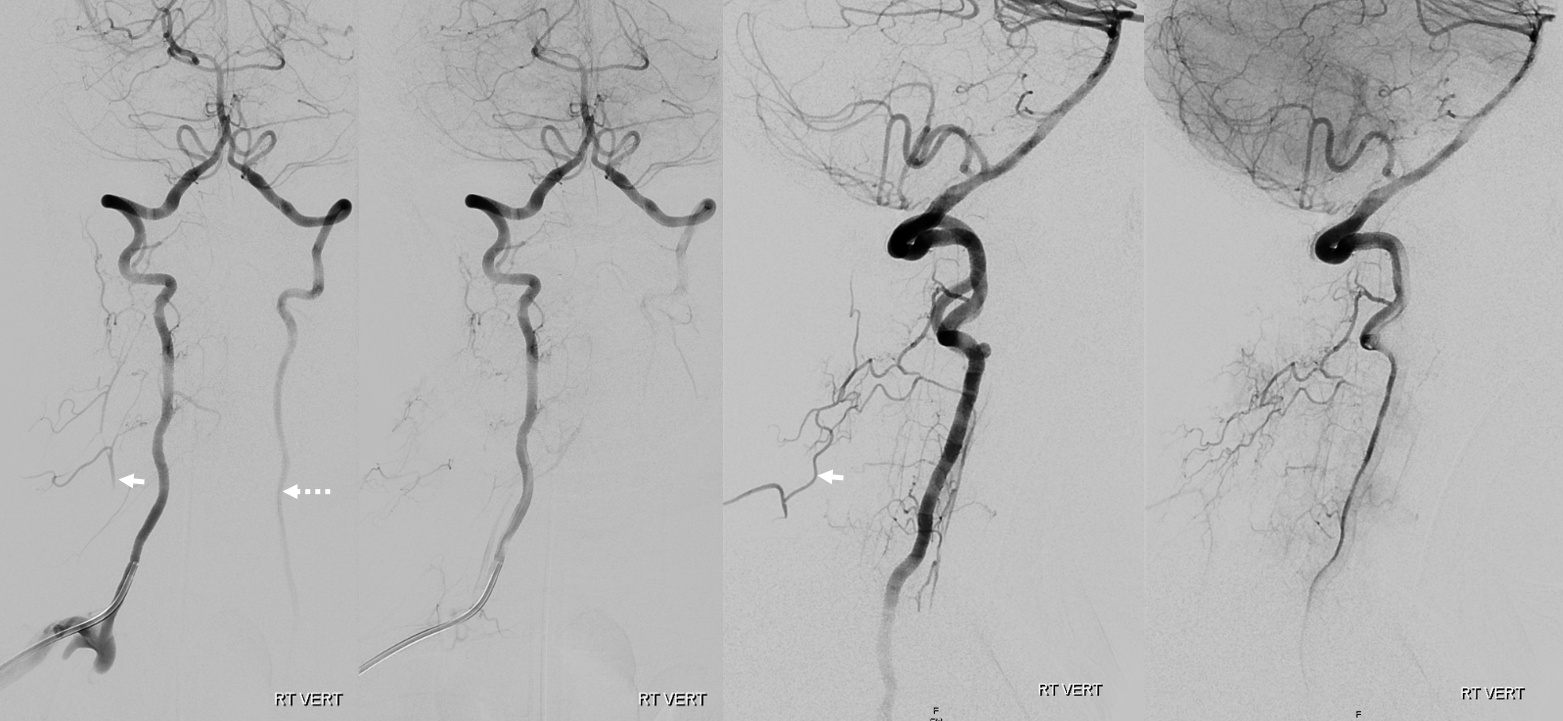
Vertebral Artery Reconstitution
Deep cervical artery is one of principal vessels that can resupply a proximally occluded vert (other candidates are occipital and ascending cervical). Usually the flow constraint is at the ostium, and is atheromatous in etiology. Mid-cervical vert occlusions are rare. Upper (C1 level) cervical vert flow problems are usually due to dissections. These usually occur above the C1 muscular branch and therefore neither deep cervical nor occipital are able to help out. However, there are exceptions. Look for example at his surfer with bilateral upper vertebral dissections. The two vessels reconstituting the upper verts (above the dissections) are deep cervical arteries. The below images are courtesy of Dr. Omar Kass Hout and Dr. Tibor Becske and are part of a cool basilar-via-PCOM thrombectomy case to be seen here
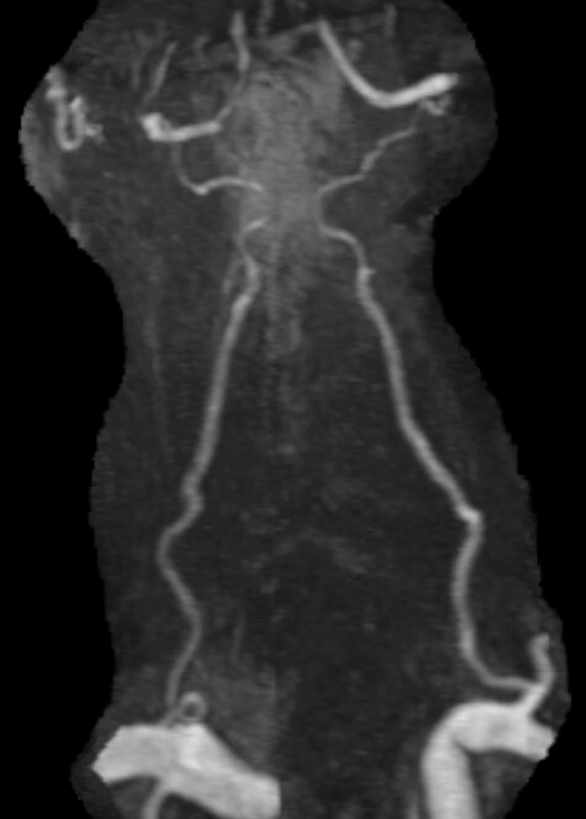
Angiography of same case
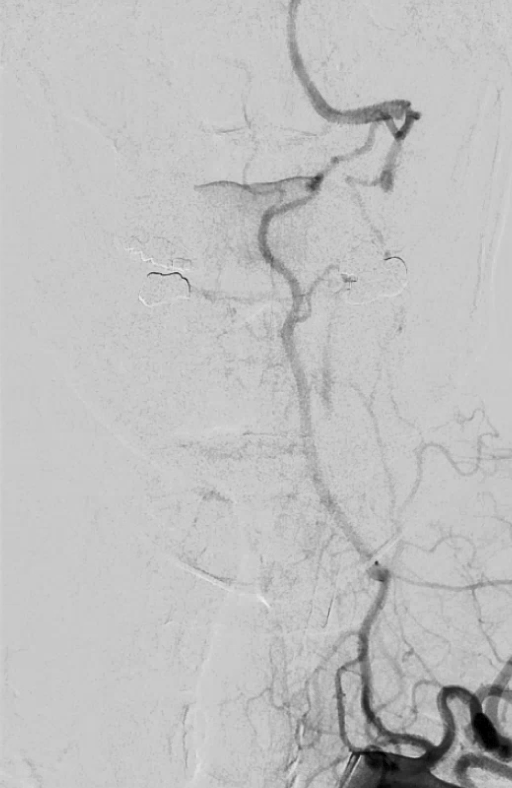
Lateral view, in case u still dont believe this is a deep cervical certical to vert reconstitution at C1 and C2 levels
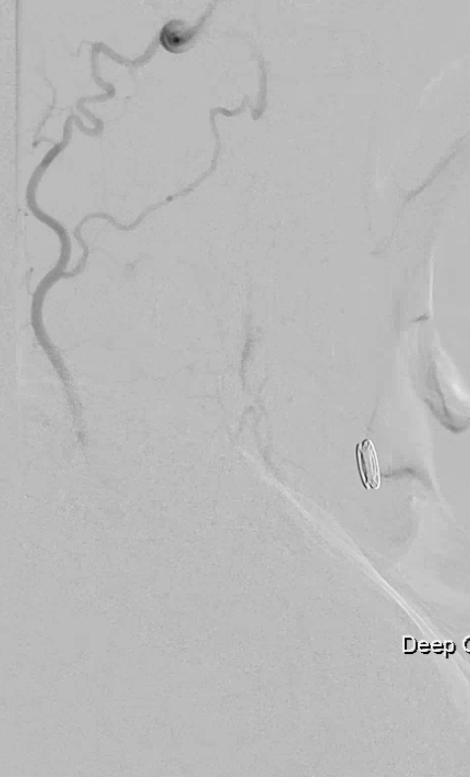
Another case, courtesy Dr. Erez Nossek
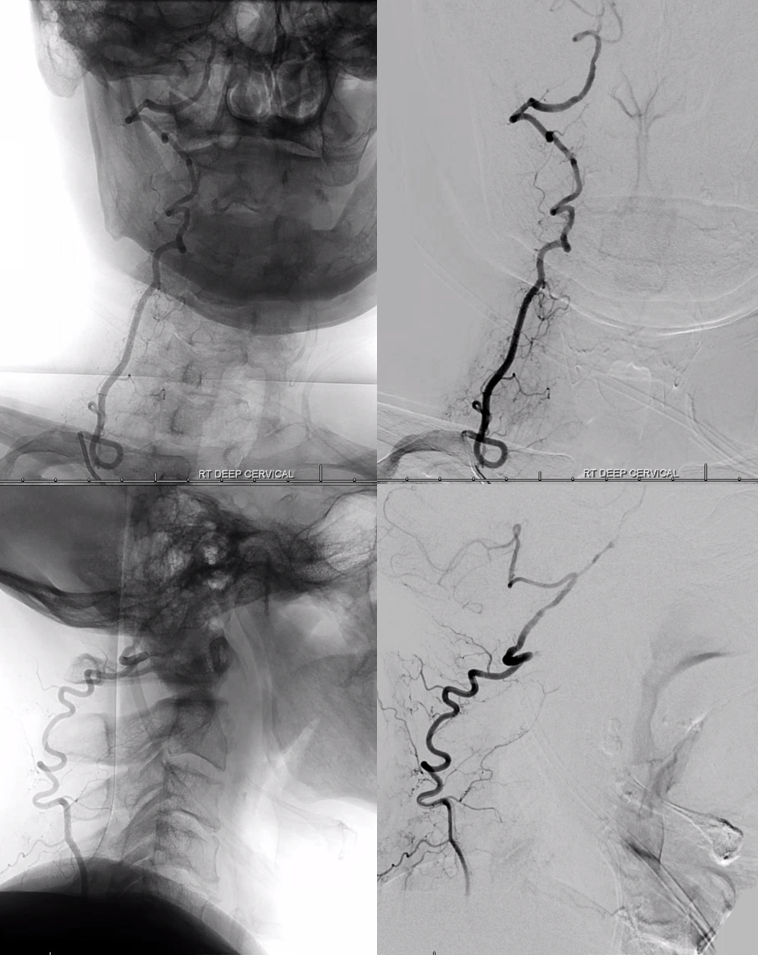
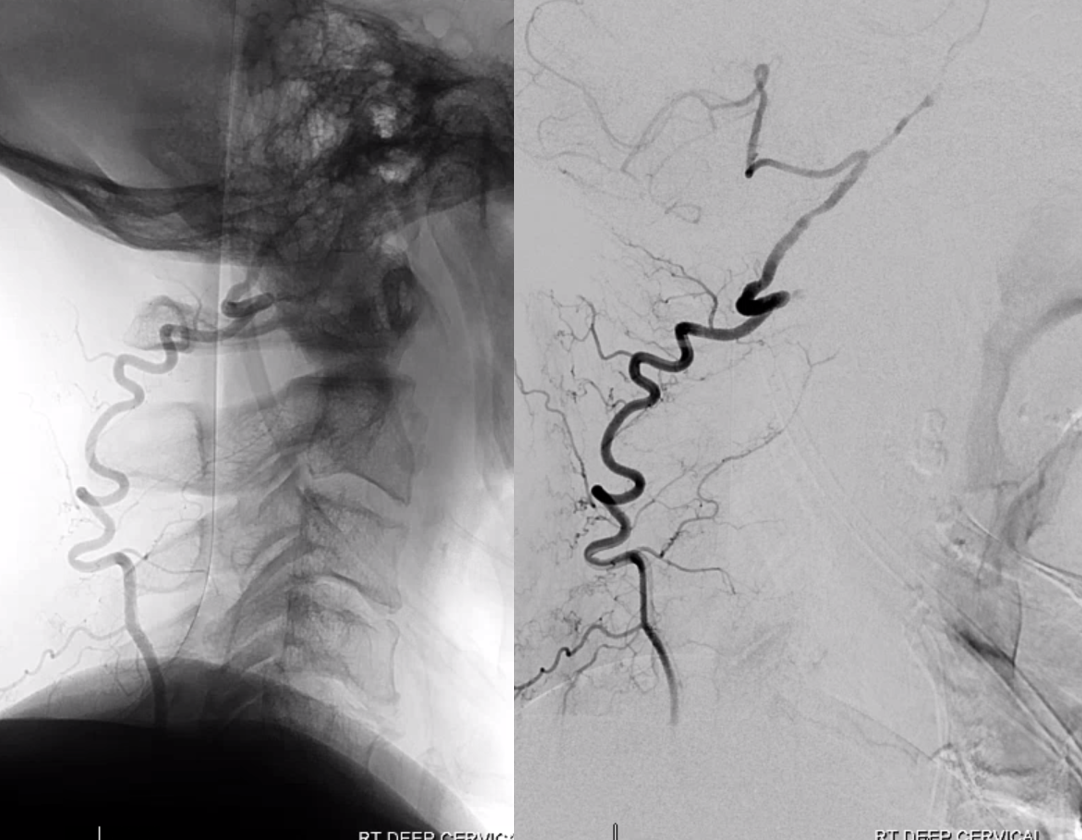
In more proximal (ostium) occlusions, both ascending cervical (orange) and deep cervical (yellow) arteries participate in vert (red) reconstitution, as seen here
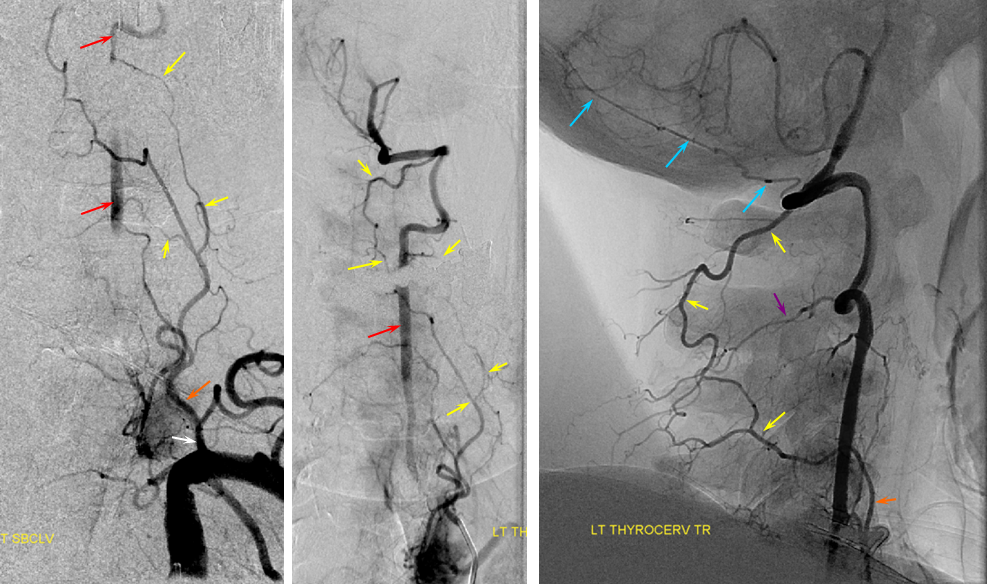
Here is another example, courtesy Dr. Eytan Raz — connections are via C3 (ball arrow) and C1 (dashed arrow) muscular branches. Vert is arrows, occipital is arrowhead. At the upper cervical segments, either deep cervical, occipital, or both can do the job.
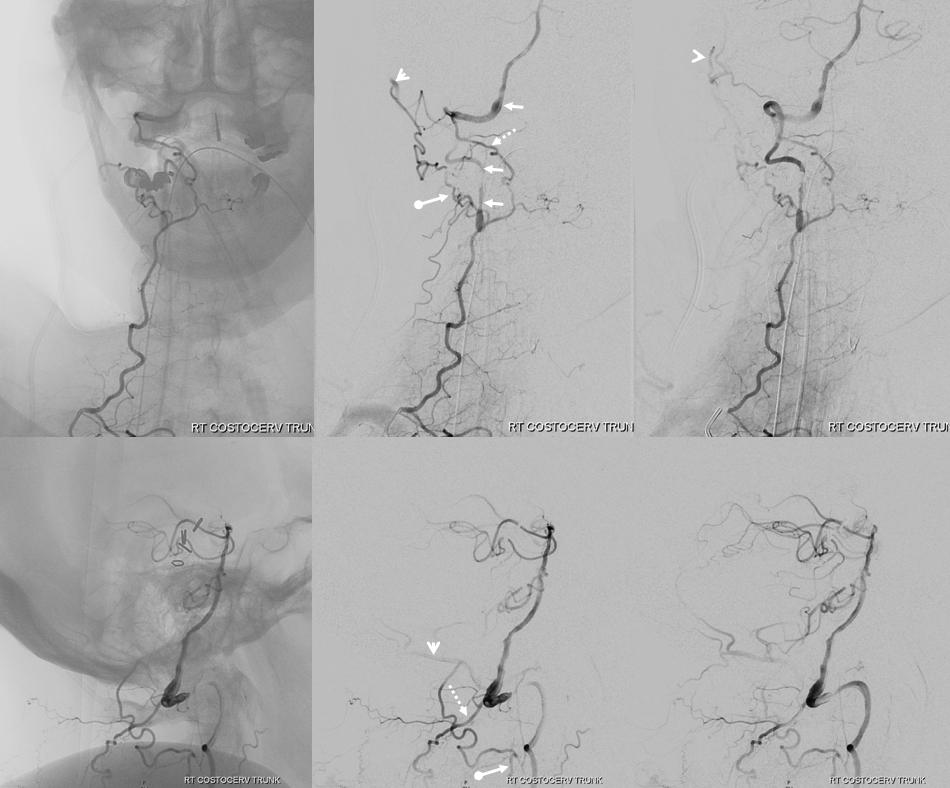
Indeed, in the same patient, injection of occipital artery opacifies the same anastomotic network seen above.
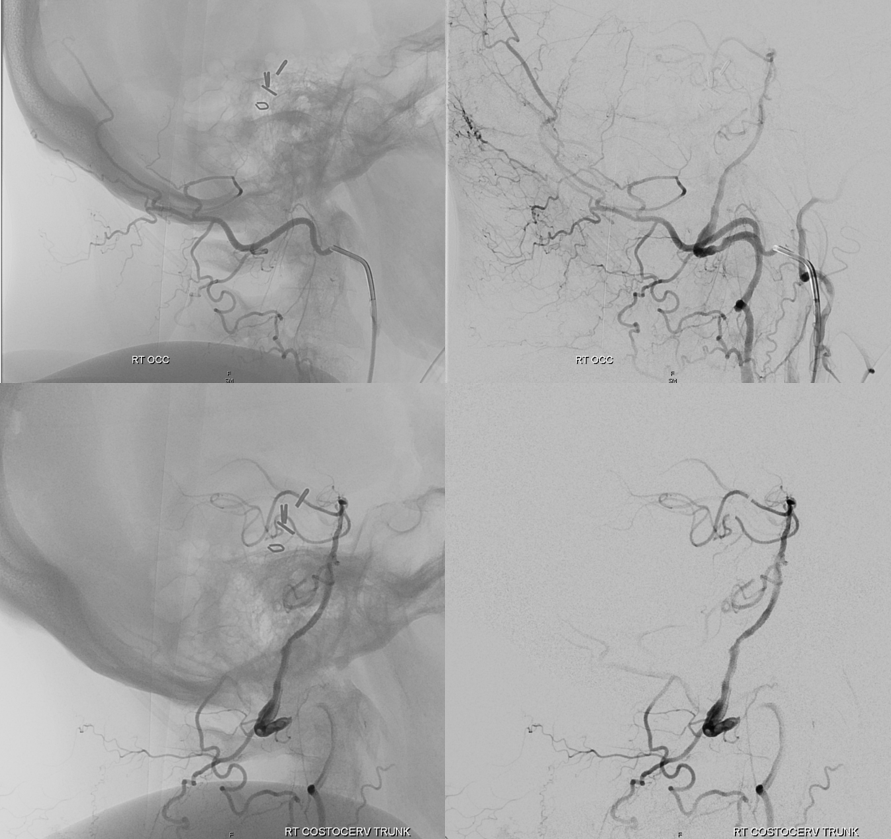
Torcular dural fistula supply
The deep cervical artery, as the vessel usually responsible for supply of midline structures such as spinous processes, extends its territory all the way to the up to cranium. It is for that reason that it will usually participate in supply of torcular dural fistulas, instead of the more lateral occipital artery (which is a transeversely oriented segmental vessel, which deep cervical is intersegmental). Here is an example
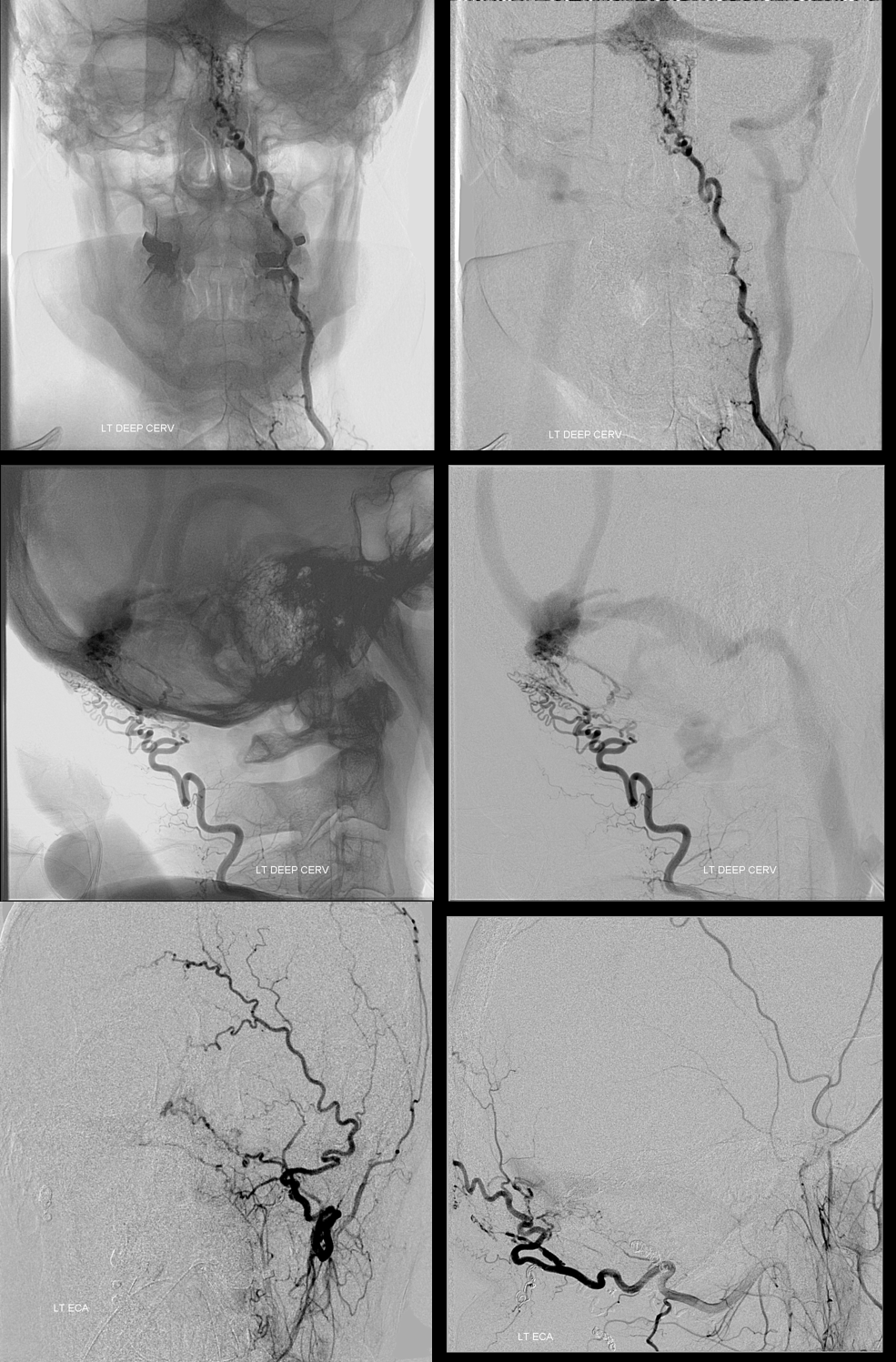
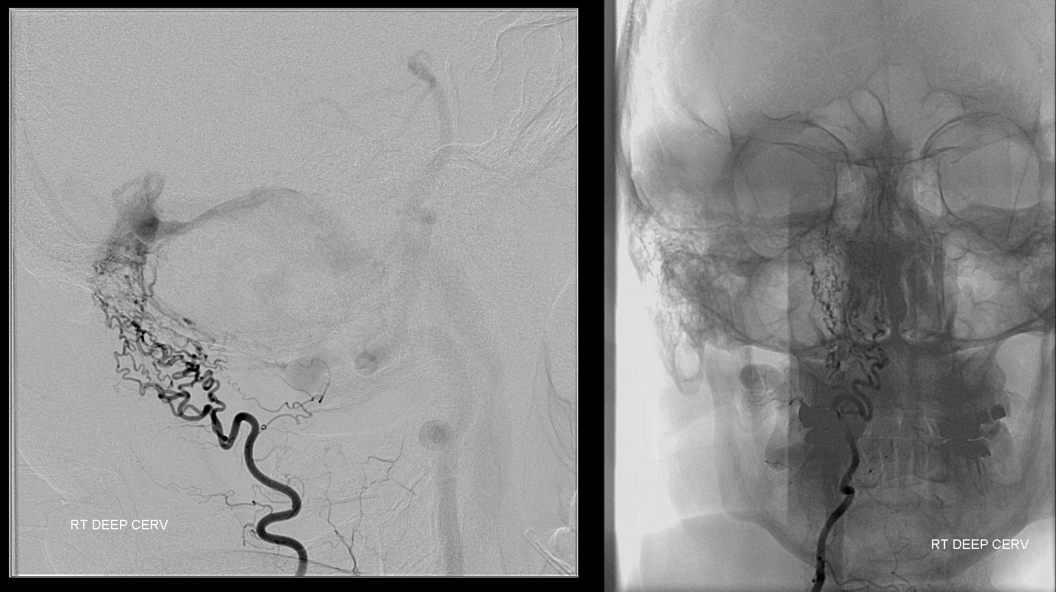
Same case, right side
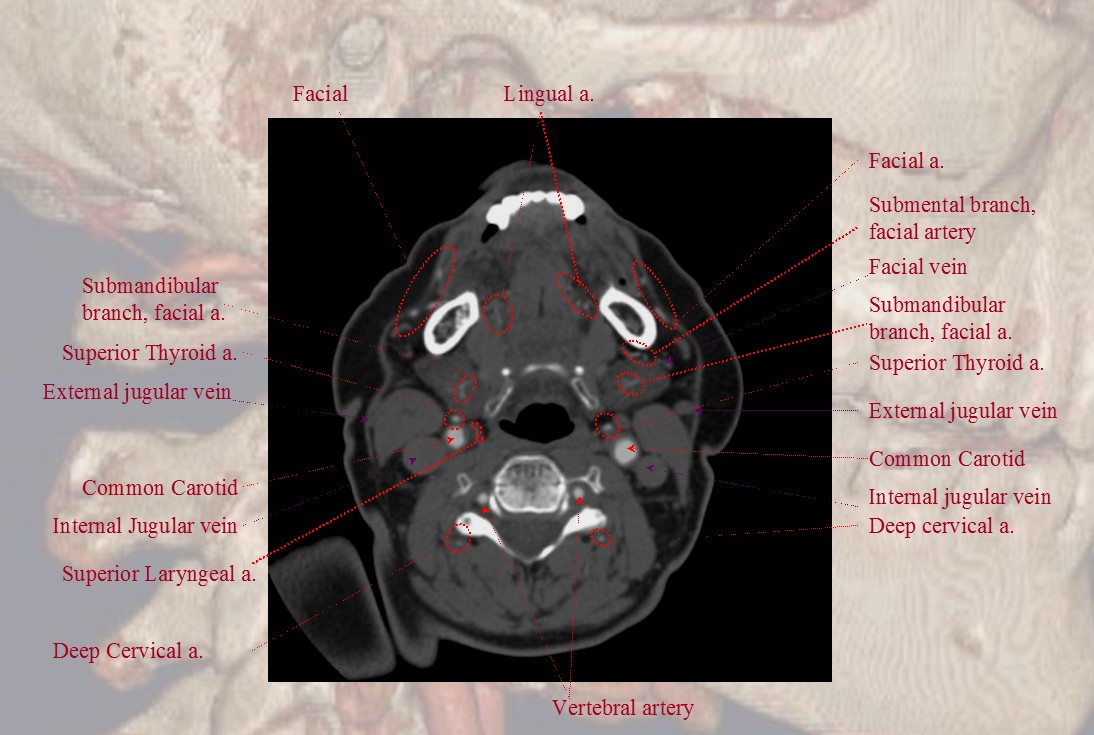
Finally, if you want traditional cross-sectional images with labels, look at our CTA Atlas Page or see below
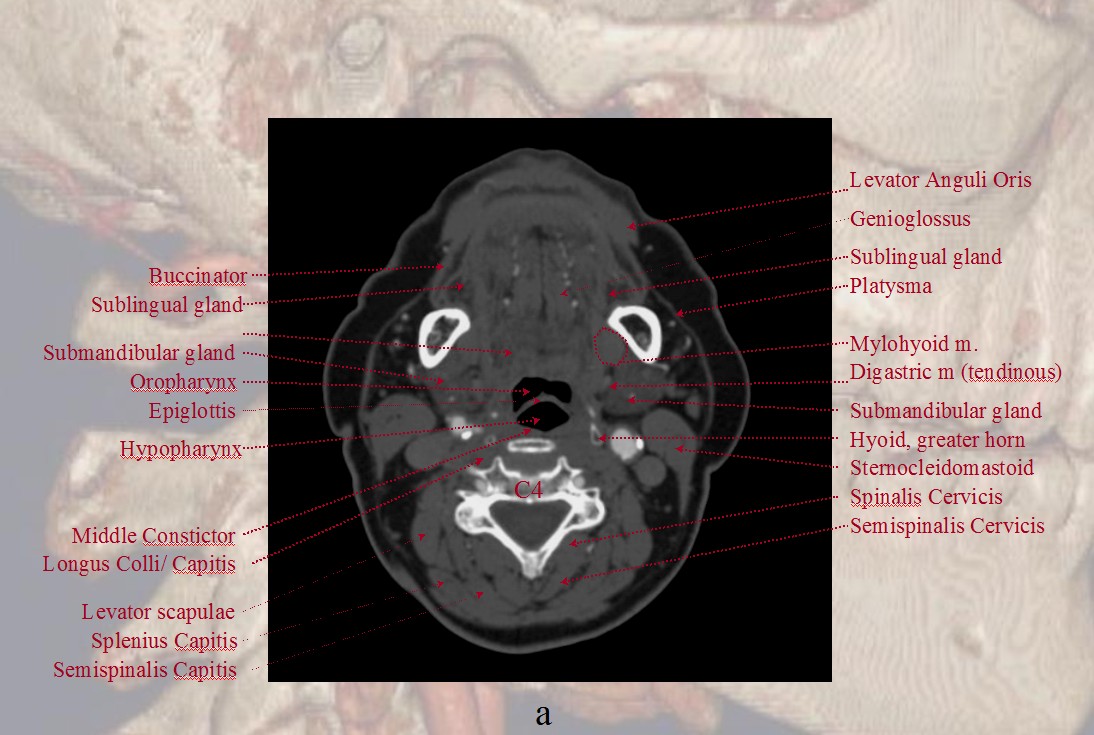
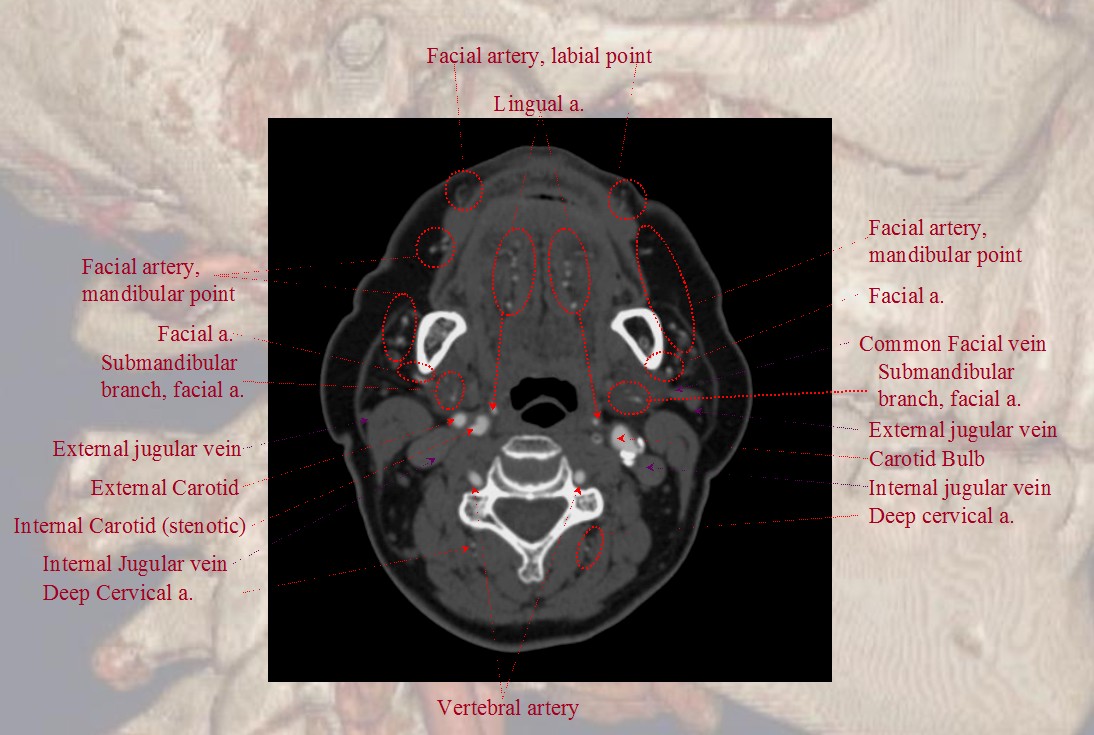
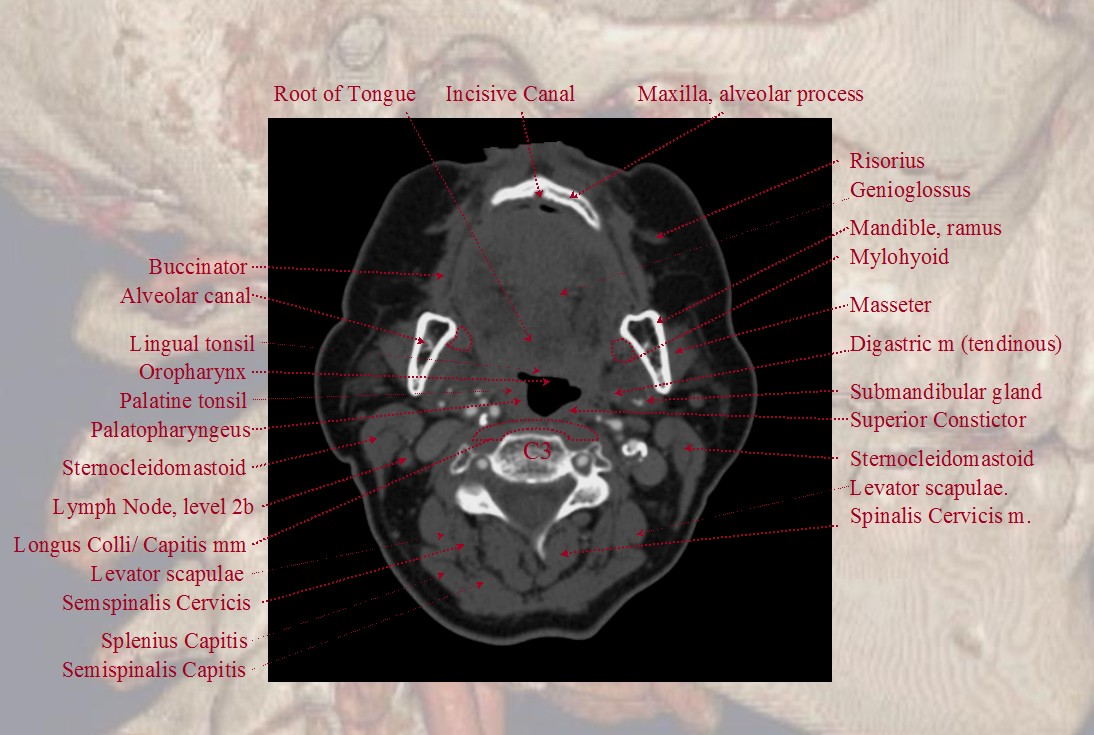
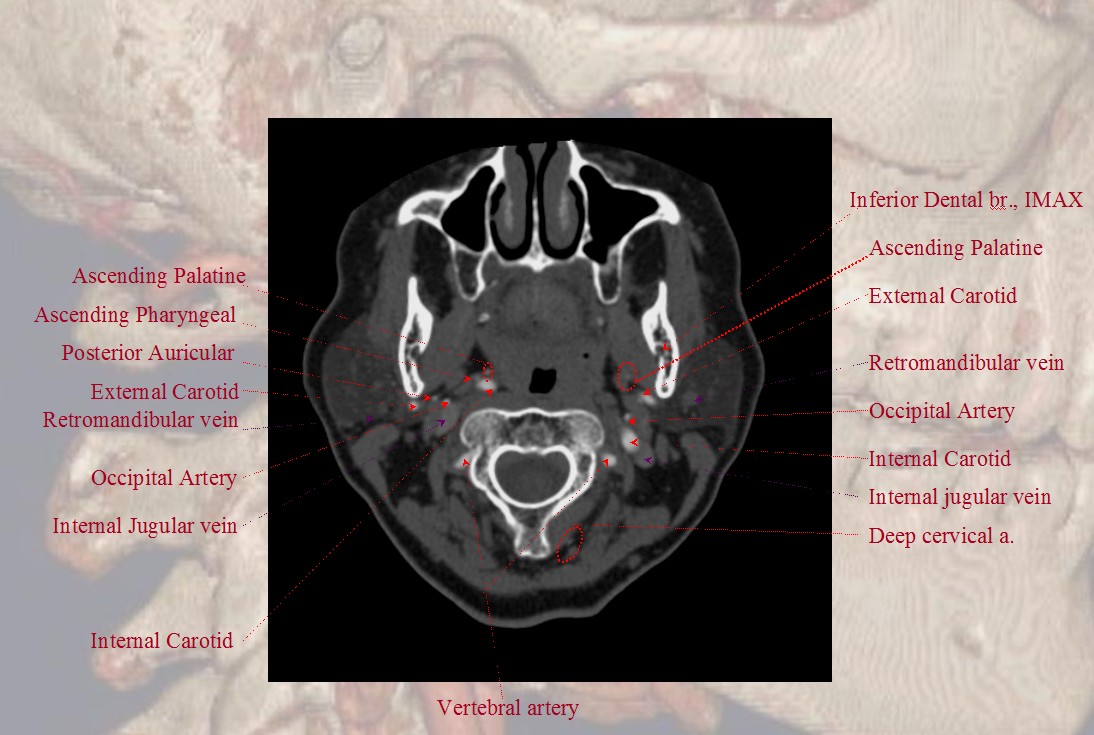
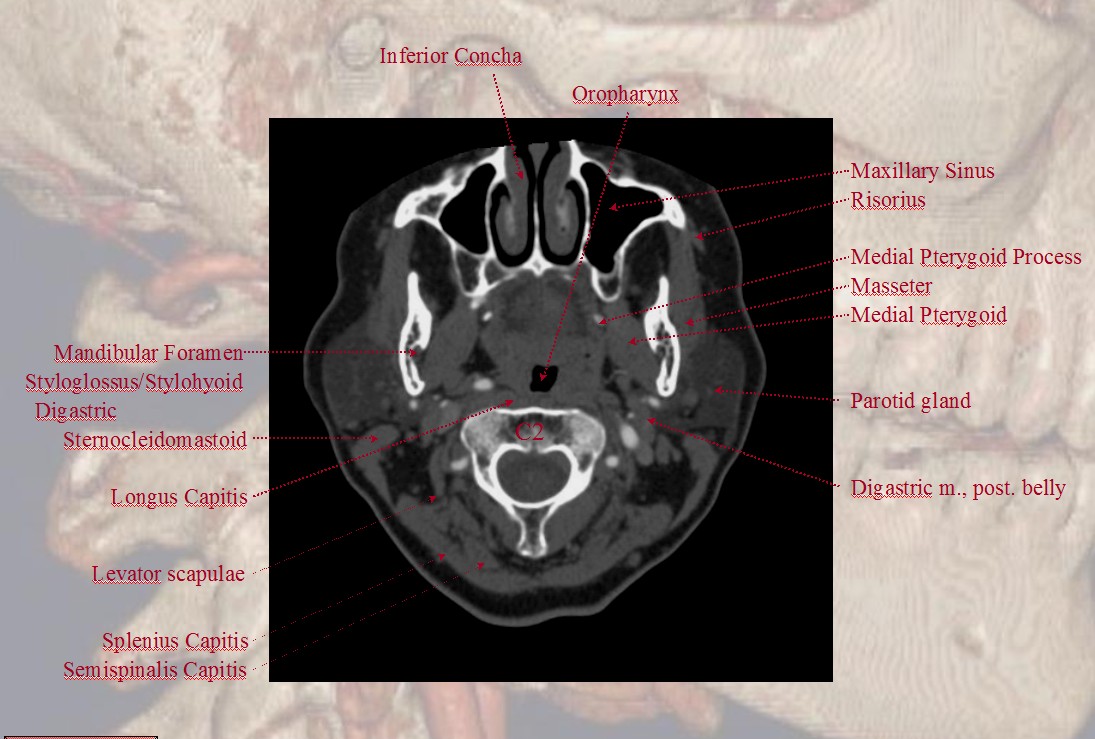
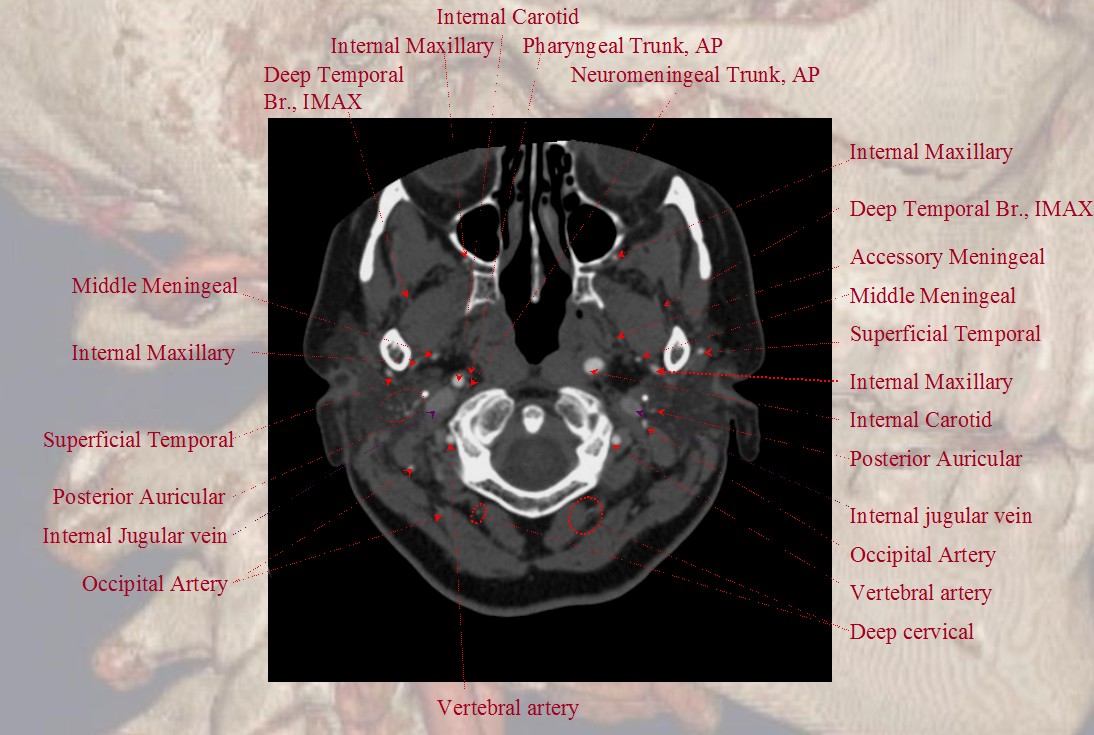
For more information, see other pages of the “Anatomy and Variants” section
