Another one of those cautionary tales. The big picture is to have a region-based rather than vessel-based approach. Meaning what? There are a myriad ways that vessels are connected to one another, and sometimes in unpredictable ways. Region-based means that if you are working near some strucutre you may or may not want to get into, there are various ways by which that might happen and so its important to be vigilant for various possibilities.
Specifically here, using liquid embolics near the orbit means that there are various possibilities for the material to end up in the orbit. Some connections may be occult, others unusual. The simple message is if you are near something, be aware. More orbit info on the ophthalmic artery page
MMA embo request post evacuation of large left subdural. Naturally, the left MMA is gone. There is a meningolacrimal branch however. and a small frontal meningeal remnant. so we coiled it…
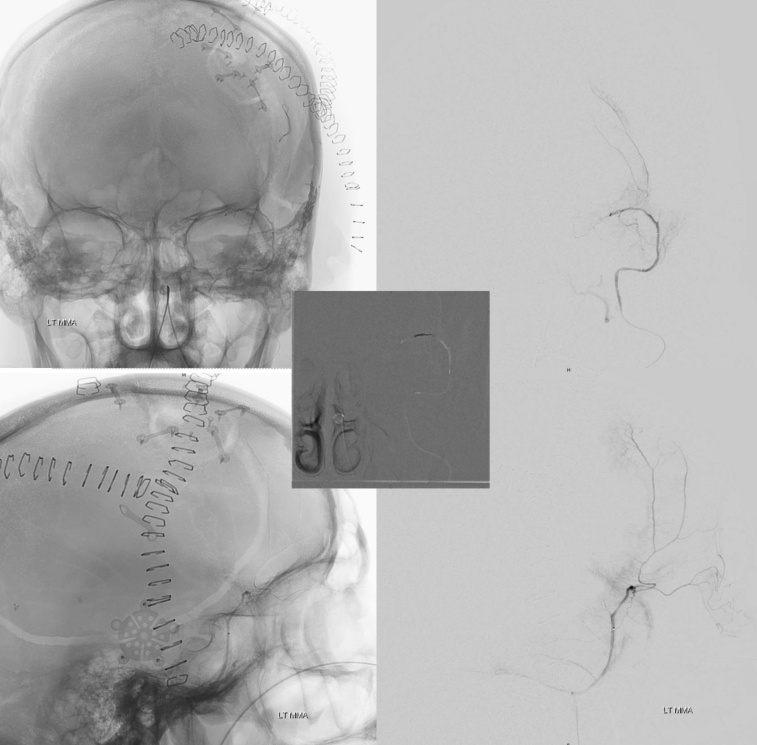
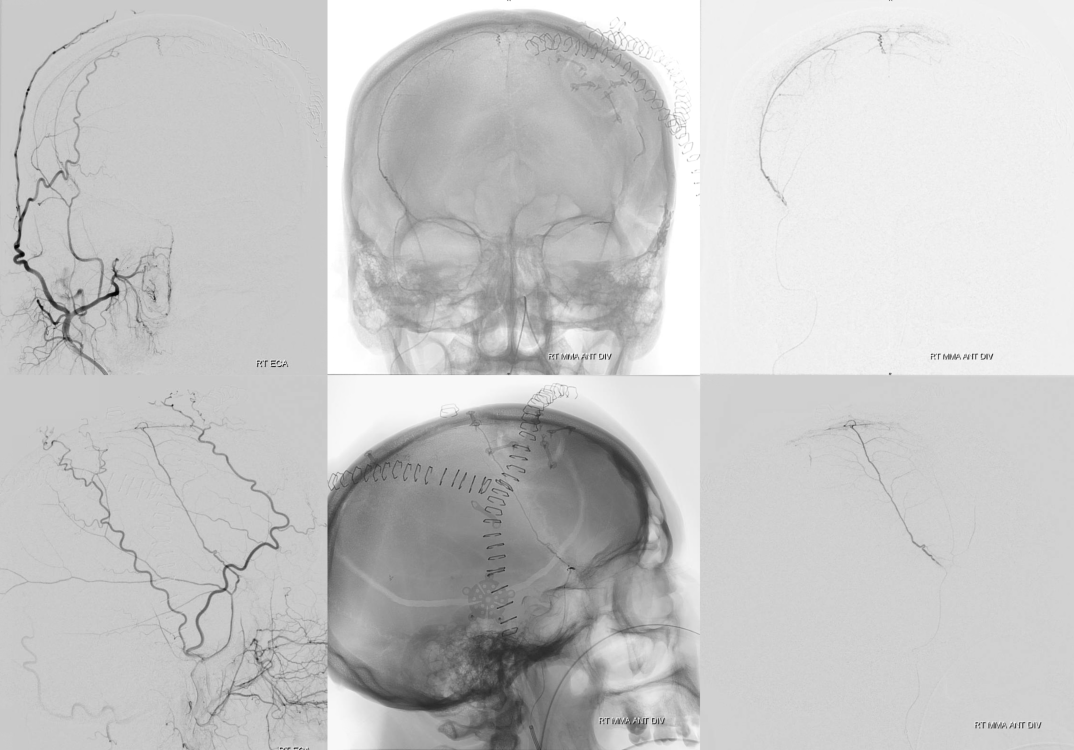
The idea is to embolize the right dura via left MMA collaterals. Images on left are ECA. On the right a Scepter C is in the anterior/frontal MMA division. Note anastomoses with left parasagittal dural convexity. There is no contrast reflux and no orbital contribution is seen from a strong wedge position injection of the Scepter. The tip is just above the orbital root — whcih means still near the orbit.
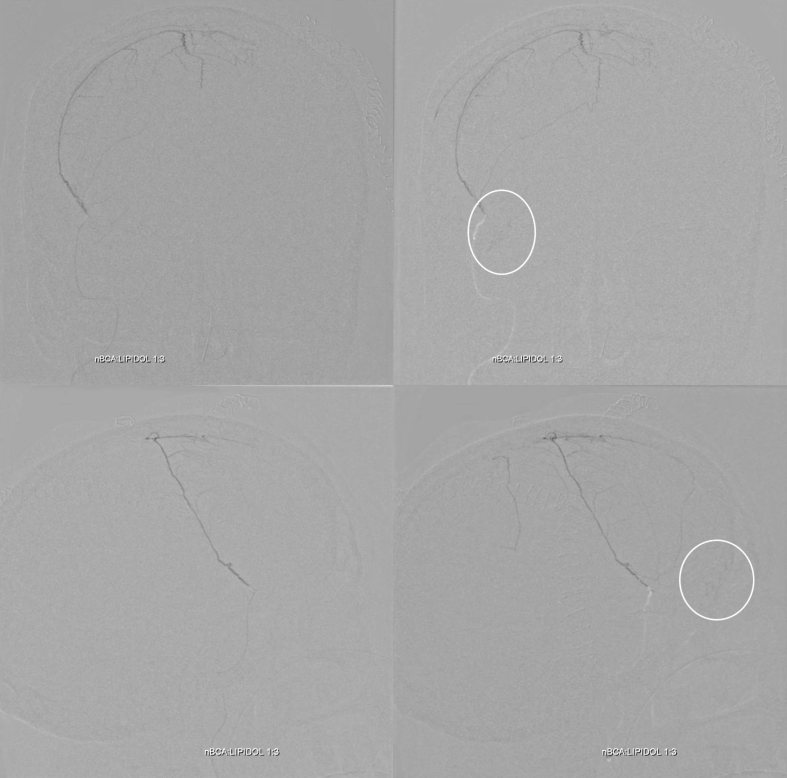
nBCA:lipidol 1:3 injection cast. See the glue in the lateral orbit? Also note the desired penetration of liquid embolic into the left parasagittal convexity and into the anterior meningeal network — thats the good thing. After seeing glue in the orbit, injection was terminated.
To understand what exactly happened, there is a DYNA CT. A small and unusual transosseous branch of the MMA re-enters the orbit from above. By this route the embolic ends up where we dont want it. There is no clinical issue since it is far away from the retinal/ciliary vessels. However, continued injection could have ended up there.
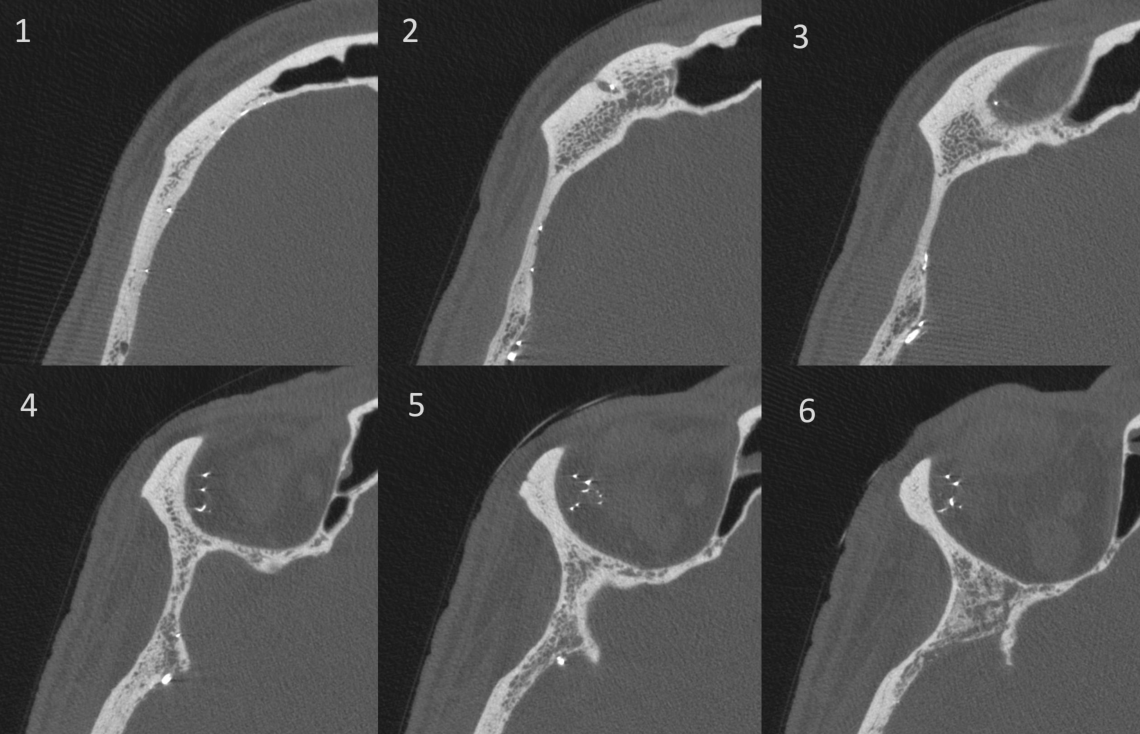
The moral is to recognize that even having catheter position above the orbital roof is not a guarantee. Near the orbit means possibly in the orbit. So be careful.
DYNA of the convexity, showing excellent penetration into left parasagittal membranes
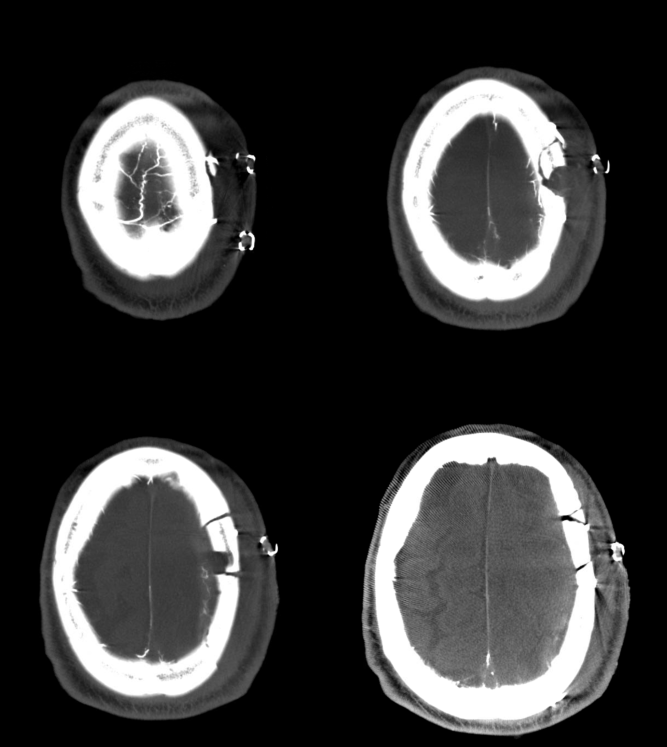
See other cases of contralateral subdural embolization on “Case Archives” page
